Key Takeaways
Managing multiple joint pain without swelling during menopause doesn’t have to be a mystery or a daily drain on your productivity. Here’s a rapid-fire summary of the most actionable insights and practical strategies you can put to work immediately—curated for tech-minded professionals who value both clarity and efficiency.
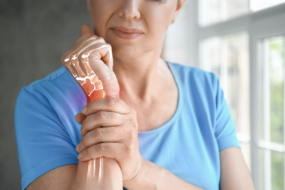
- Recognize non-inflammatory joint pain as a common menopause symptom—aches and stiffness without swelling often affect hands, knees, hips, and back, shifting throughout the day.
- Rule out red flags early—visible swelling, intense morning stiffness, or severe pain signal the need for medical attention; don’t ignore signs that fall outside the “usual” menopause experience.
- Hormonal changes drive discomfort—the drop in estrogen during menopause reduces joint lubrication, leading to that “creaky hinge” sensation, especially after inactivity.
- Optimize your daily routine with movement—short, low-impact activities like walking, stretching, and “movement snacks” every 30–45 minutes can dramatically reduce joint stiffness.
- Prioritize strength and flexibility—even brief strength training sessions (2–3 times a week) and five-minute stretching routines can offload joints and restore mobility.
- Leverage technology for self-care—use symptom tracking apps, wearables, or AI workflows to monitor patterns and prompt movement, making on-the-go tracking effortless.
- Sleep and stress management power pain relief—quality sleep routines and mindfulness practices can cut pain sensitivity by up to 32%, acting as a “software upgrade” for joint comfort.
- Personalize your strategy with expert input—tailor your approach with a clear symptom history and seek advice on tools like hormone therapy, supplements, or physical therapy as needed.
Small, strategic shifts—and smart use of tech—put you back in control of menopausal joint pain. Dive into the full article for deeper, tailor-made solutions to keep you moving and thriving.
Introduction
Ever notice your knees or hands feel stiff and achy—yet there’s no visible swelling or redness in sight? You’re not alone. For tech-driven professionals navigating menopause, unexplained joint discomfort can sneak in like an unscheduled software update: subtle, persistent, and impossible to ignore.
It’s tempting to wonder, is this normal—or should I be worried? As hormones shift, up to 60% of women report joint aches during menopause, often without any classic signs of arthritis. You might feel “creaky” standing up from your desk or need a few extra steps to shake off morning stiffness—yet your joints look perfectly normal.
Here’s why this matters for busy professionals:
- Misreading symptoms often triggers unnecessary doctor visits, anxiety, or even the wrong medications
- Recognizing the true pattern means fewer distractions and targeted, real-world solutions
- Knowing when to track and when to escalate helps you manage health like everything else: efficiently and on your terms
The good news? Today’s combination of science-backed lifestyle tweaks and smart tech puts control firmly in your court. From bulletproof movement routines tailored for desk life, to quick “check-engine” tips you can run with your smartwatch, practical answers are closer than you think.
What’s inside? You’ll learn:
- Spotting the subtle differences between menopause-related joint pain and conditions that actually require urgent care
- Proven strategies—movement, workspace hacks, symptom tracking, and digital nudges—for real relief
- Clear guidelines on when it’s time to involve your doctor, versus when self-care truly pays off
Think of it as an upgrade for your daily comfort: a toolkit built for those who want actionable insight, not just reassurance.
Ready to see what’s actually happening beneath the surface—and how to manage multiple joint aches gracefully? Let’s pull back the curtain and decode why these invisible pains show up during menopause, and what you can do next.
Understanding Multiple Joint Pain Without Swelling in Menopause
Menopause often introduces aching, stiffness, or discomfort in multiple joints, even when there’s no visible swelling, redness, or heat. This can feel like a dull, persistent soreness—picture waking up stiff, or feeling “creaky” after long periods at your desk, but without any joint looking puffy or inflamed.
Unlike autoimmune or inflammatory arthritis (like rheumatoid arthritis), menopausal joint pain isn’t accompanied by obvious signs of inflammation. There’s no joint warmth, significant redness, or swelling. The pain pattern is more about sensation than what you see.
Where Does Non-Swelling Joint Pain Typically Strike?
The most commonly affected areas are:
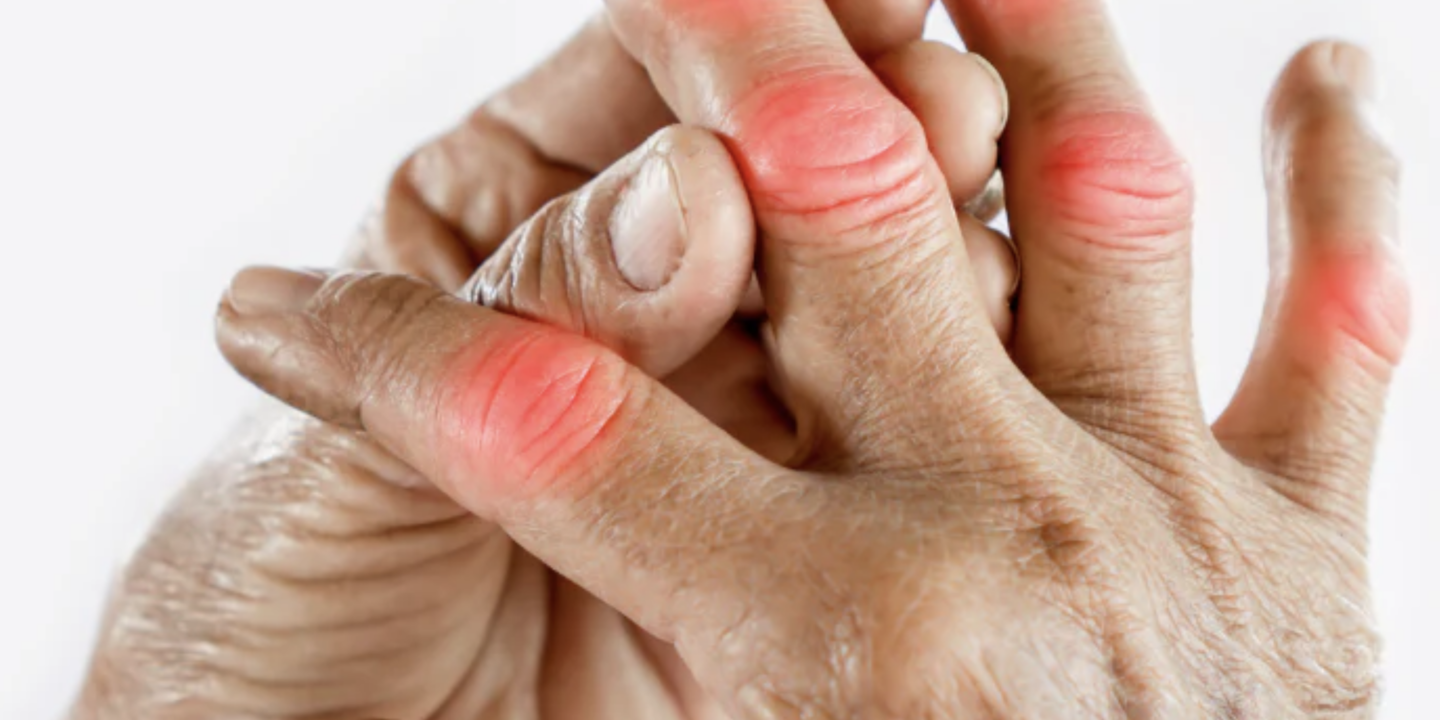
- Hands and fingers: Sore knuckles, weak grip, or mild clicking
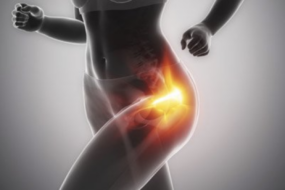
- Knees and hips: Ache after standing or climbing stairs
- Shoulders and neck: Tightness, limited range if you sleep awkwardly
- Lower back: Stiffness after sitting, not sharp pain
You might notice the pain is:
- Worse in the morning or after inactivity, but gradually improves as you move (“rusty hinge” effect)
- Tends to shift from joint to joint or affects several places at once
- Feels more like stiffness, soreness, or a dull ache than sharp, burning, or intense pain
How Do You Recognize This? Real-World Scenarios
Imagine you wake up feeling like your hands are “full of sand,” or after a long session at your computer, your knees take several steps to “wake up.” There’s no swelling, but the daily grind is real. This is menopausal non-inflammatory joint pain—common, but often invisible.
Diagnosing this pattern matters:
- Incorrectly assuming it’s arthritis can lead to unnecessary worry, doctor visits, or medications
- Accurate recognition means you can focus on what actually works—lifestyle shifts, appropriate relief, and the right support
Why Does Naming the Pattern Matter?
Knowing your joint pain isn’t caused by swelling or active inflammation allows you to:
- Rule out more concerning conditions early
- Prioritize evidence-based self-care strategies (like movement and ergonomics)
- Communicate clearly with your doctor, saving both time and worry
“Not all joint pain needs an urgent solution—but every case deserves a smart strategy.”
Picture this: You trade uncertainty for a plan tailored to non-inflammatory pain, setting yourself up for real relief and fewer false alarms. When you know what you’re dealing with, you can move confidently to solutions that fit your lifestyle.
Why Does Joint Pain Without Swelling Happen During Menopause?
Hormonal Shifts and Their Musculoskeletal Ripple Effect
Menopause brings a steep drop in estrogen—a hormone with a starring role in joint health.
Estrogen keeps joints slippery by maintaining cartilage and boosting synovial fluid. When levels plummet, joints lose their built-in protection, often resulting in:
- Stiffness and diffuse aches that move from one joint to another
- Early-onset “wear and tear” (osteoarthritis) especially in hands, knees, and hips
- Worsening pain after rest, even without swelling or heat
Imagine estrogen as your body's built-in anti-rust spray for joints. When it’s gone, the “squeak” is real—just quieter than classic arthritis.
Quotable: “When estrogen drops, your joints lose their built-in ‘anti-rust’—making every day a bit creakier, even without swelling.”
Muscles, Tendons, and Ligaments: The Silent Victims
It’s not just joints; sarcopenia, or muscle loss, accelerates during menopause.
Combine this with less-flexible tendons and stiffer ligaments and you get:
- Hip/gluteal “bursitis” pains and shoulder twinges without visible inflammation
- Achilles soreness after walking or exercise despite normal-looking ankles
- A generalized feeling of “being less springy” during daily movements
These subtle changes mean your joints work harder without back-up support, making discomfort far more noticeable.
Quotable: “Menopause makes your muscles and tendons less forgiving—cue joint pain, even when everything looks perfectly normal.”
Lifestyle Factors: The Double Whammy
Tally up extra pounds and more time spent sitting, and you have a recipe for amplifying joint pain.
- Inactivity decreases synovial fluid flow, stiffening joints
- Weight gain means knees, hips, and the lower back work overtime
Picture this: your joints are “moving parts” that need their weekly ‘oil change.’ No movement means no lubrication, more friction, and increased discomfort.
Quotable: “Sitting too long? It’s like letting your joints run dry—minimal movement means maximum stiffness.”
Central Sensitivity, Sleep, and Mood: Pain’s Hidden Drivers
Add in poor sleep, stress, and shifting moods—all hallmarks of menopause—and you alter how your brain processes pain.
- Disrupted sleep can make minor aches feel major
- Stress and anxiety lower your pain threshold
- Sometimes, what you’re feeling is a “pain signal” from the nervous system, not actual joint damage
If you’re tossing and turning at 2 a.m., don’t be surprised if joint pain tags along the next day.
Recognizing that joint pain without swelling during menopause is multi-factorial is step one. With this awareness, you can target the root causes—hormones, muscle changes, habits, and even sleep—to regain flexibility and comfort in your day-to-day life.
Ruling Out Other Causes: When Pain Needs a Closer Look
Red Flags That Shouldn’t Be Ignored
Not every ache or stiffness is “just menopause.” Some symptoms demand immediate attention. If you notice any of the following, don’t wait—reach out to a healthcare provider right away:
- Visible joint swelling, redness, or warmth (signals possible infection or inflammatory arthritis)
- Prolonged morning stiffness—lasting more than 30 to 60 minutes
- Unexpected weight loss or persistent fever
- Unexplained rash or new severe fatigue
- Joints that suddenly become deformed or change shape
- Sudden, severe joint pain (especially in one joint)
- Very localized pain after a fall—especially with osteoporosis risk
Each of these flags points to something more serious than menopausal joint pain—think of them as your body’s “do not ignore” alerts.
“When in doubt, check it out—peace of mind is always worth it.”
The Diagnostic Process
So, what happens if you go in for an evaluation? Your doctor’s job is to separate classic menopause joint pain from other diseases. This isn’t a guessing game—it’s a methodical process that might include:
- History check: When did the pain start? Which joints? Any swelling, redness, or heat?
- Physical exam: Your provider will look for visible signs—do joints look normal, or is there visible swelling?
- Blood tests to check for:
- Inflammatory markers (like ESR, CRP)
- Thyroid function
- Vitamin D and calcium levels
- Autoimmune screens (if needed)
- Imaging:
- X-rays to spot early arthritis or significant wear
- Ultrasound to check for unseen inflammation or fluid
If you have a family history of autoimmune conditions or risk factors for osteoporosis, your workup may dig deeper. Nearly 20% of women over 50 develop arthritis, so clinicians look for patterns—not just one symptom.
Imagine sitting in your doctor’s office with a clear bullet list of symptoms, timeline, and risk factors—this “cheat sheet” approach can speed up diagnosis and the path to relief.
If you’re on the fence about a symptom, remember: “Asking early beats worrying late.” A quick professional check saves you both needless anxiety and the risk of missing something urgent.
Thorough symptom tracking and a proactive mindset keep you in the driver’s seat—your health data is as crucial as any app or workflow in your digital toolkit. If something doesn’t fit the typical menopause story, trust your instincts and get it seen.
Effective Management Strategies for Multiple Joint Pain Without Swelling
Medical Review and Personalization
Navigating joint pain with zero swelling means personalized assessment is your starting line.
Keep an eye on symptom changes and communicate trends to your provider—think: “pain’s worse after sitting,” or “stiffest in the morning, better after moving.”
Picture this: you walk into your appointment with a list of which joints hurt, time of day it spikes, and any triggers you’ve noticed. Clear reports lead to better care and faster solutions.
Lifestyle and Physical Approaches
Think of your joints as moving parts in a machine—they do best with regular, gentle use.
Here’s your maintenance checklist:
- Low-impact cardio: Walking, swimming, cycling, yoga, or Pilates 4–5x/week boosts lubrication and cuts stiffness.
- Movement snacks: Stand up, stretch, or move every 30–45 minutes to keep discomfort at bay.
“A five-minute walk every hour keeps pain from becoming the boss of your day.”
Muscle Strengthening and Tendon Support
Stronger muscles = less joint stress. Squeeze in:
- Strength training: 2–3 sessions/week, even if it’s just resistance bands or bodyweight.
- Focus on hips, thighs, shoulders, and core for maximum relief.
Busy day? One quick miniband circuit while waiting for your coffee is real-world innovation.
Mobility, Stretching, and Ergonomics
- Daily stretching: Just 5 minutes targets stiffness and boosts mobility.
- Work/home tweaks: Adjust chair height, use a footrest, or swap to an ergonomic mouse.
Little improvements in how you move and sit add up—especially at the desk.
Weight, Sleep, and Stress
Just a 5% drop in body weight can take thousands of pounds of pressure off your knees each year.
Upgrade your sleep with:
- Consistent bedtimes and no screens an hour before (yes, it’s tough, but worth it).
- Meditation or deep breathing to dial down pain amplification from stress.
“Better sleep is the secret software update your joints are begging for.”
Thermal Therapies and Quick Relief
Reach for a warm bath or heating pad for morning stiffness. Ice packs soothe after extra-busy days.
Heat and cold: Old-school, still unbeaten for short-term joint comfort.
Medications and Supplements: Facts First
What works when?
- NSAIDs or acetaminophen: Short-term boosts during flares (only if doctor okays it).
- Topical NSAIDS: Try gel on knees or hands for fewer side effects.
- Supplement with vitamin D/calcium if you’re low. Glucosamine/chondroitin? Your mileage may vary.
Natural remedies can help, but set realistic expectations over miracle results.
Navigating Menopause Hormone Therapy (MHT/HRT)
- HRT can reduce menopausal joint pain for some.
- Not everyone’s a candidate—history of cancer, clot, or heart issues matter.
- Data: Modern HRT cuts joint pain for 30–60% of users, but consult a menopause specialist for risks/benefits.
Targeted Rehabilitation and Support
Sometimes teamwork wins:
- Physiotherapy: You’ll learn custom moves for your pain pattern—think posture hacks, tendon fixes.
- Occupational therapy: Get tips for joint-protecting daily habits and workspace adjustments.
For back, hips, or pelvis: Pelvic floor workouts and micro-adjustments in how you sit/stand can make a real difference.
Advanced procedures—like injections or surgery—are rare, but your care team can guide you if symptoms persist.
The right routine—customized by your real-world needs and lifestyle—brings relief you can feel and track. Smart tweaks, daily movement, and expert advice put you back in the driver’s seat, even if discomfort tries to steal the wheel.
Living Well With Menopausal Joint Pain: Real-World Tips and Future Innovations
Managing joint pain during menopause — especially when there’s no visible swelling — doesn’t have to eat up your entire schedule. Practical self-management strategies fit naturally into even the busiest tech-professional lifestyle.
Instead of chasing endless “miracle cures,” start with what drives results:
- Daily, low-impact movement: Aim for 10-minute “movement snacks” at your desk or between meetings — walking, doorway stretches, or hip circles all count.
- Strengthen, don’t just stretch: Think two brief muscle-building sessions a week (bodyweight squats or resistance bands while your coffee brews).
- Optimize your workspace: Adjust your chair/desk to support posture. Try a standing desk for an hour daily to cut back stiffness and keep circulation flowing.
“Every movement is a vote for less stiffness tomorrow.” That's not just catchy—research shows that short bursts of motion reduce discomfort more than periodic, intense exercise.
Streamlined Tracking and Lifestyle Hacks
Your phone can be your best self-management ally. Downloadable tools let you skip the guesswork:
- Symptom tracking apps: Tools like Bearable, PainScale, or even a color-coded Excel spreadsheet quickly highlight what’s working — and what’s not.
- Wearables: Use your smartwatch’s reminders to sneak in those movement breaks or track nightly sleep (which directly affects pain tolerance).
- AI-powered planners: Literally set up a workflow to chart your pain trends vs. activity levels in seconds.
“Small digital nudges can deliver big physical relief.” The right tech means you’re always one tap away from a clearer pattern—and better choices.
Optimism, Realism, and What’s Next
Here’s the straight talk: Menopausal joint pain is highly manageable with the right toolkit, but there’s rarely an overnight “fix.” Stay realistic yet optimistic.
Tech-savvy strategies that deliver rapid results include:
- Batch-prepping healthy lunches to manage weight and inflammation on autopilot
- Mindfulness apps reducing stress levels, proven to cut pain intensity by up to 32%
- Routine sleep optimization: Blue-light blockers, evening wind-down timers, or white noise can dramatically improve restorative sleep
Look ahead: Researchers are piloting injectable cartilage boosters and smart insoles that monitor and prompt joint-sparing moves. Picture a future where AI flags problematic activities before pain spikes.
Menopausal joint pain doesn’t control your day unless you let it. Build habits around tiny, trackable actions — and let both science and smart tech do the heavy lifting.
Takeaway: The most effective way to thrive with menopause-related joint pain is to combine bite-size movement, digital organization, and a realistic mindset. Your daily “micro-adjustments” matter far more than any single dramatic change.
Conclusion
You don’t have to let joint pain without swelling dictate your day—menopause is challenging enough without invisible aches slowing you down. Recognizing this pain for what it is means you can skip unnecessary worry and instead put evidence-based relief in the spotlight.
Small, targeted shifts in how you move, track, and adapt can quickly translate into greater comfort and control. You deserve practical, tech-empowered options that fit your routine—not one-size-fits-all solutions.
Put these insights to work today:
- Prioritize movement: Build in “mini motion sessions” throughout your workday—think five-minute walks or dynamic stretches every hour.
- Leverage technology: Use symptom tracking apps or wearables to identify patterns, goals, and what works best for your body.
- Upgrade your environment: Adjust desk setup or seating to align with ergonomic best practices for less joint fatigue.
- Layer in strength: Add two muscle-building sessions per week to boost joint stability and function.
- Refine your sleep routine: Commit to screen-free bedtime habits and track your rest for next-level pain resilience.
Ready to take the next step?
- Audit your current daily habits—pinpoint one change you’ll make this week, whether it’s a new ergonomic chair, a recurring stretch reminder, or committing to a digital symptom journal.
- Share your plan with a colleague or accountability buddy for instant feedback and extra motivation.
- If symptoms persist or veer outside the expected menopause pattern, connect with your healthcare provider for a personalized action plan.
The future is wide open: With each small, intentional tweak, you reclaim flexibility and confidence—both in your body and your routine.
Every micro-move you make is a message to your joints: “We’re in this together, and we’re moving forward.”