Key Takeaways
If you’re busy but want real answers for managing blackheads and whiteheads, these practical insights will give you a fast, confident handle on comedonal acne. Scan these essentials to quickly learn the “why” and the “how”—so you can start smoothing your skin and streamlining your routine today.
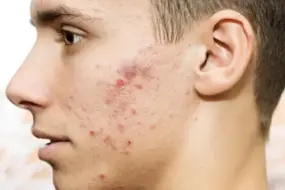
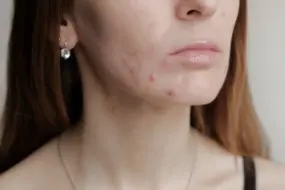
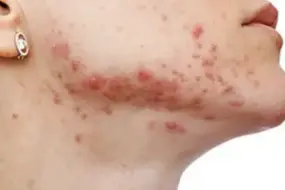
- Comedonal acne is an early-stage, non-inflammatory issue—characterized by clogged pores (blackheads and whiteheads), not redness or swelling.
- Blackheads result from open pores where oil and dead skin oxidize with air, while whiteheads have closed pores that trap material beneath the skin—think “traffic jam,” not “dirt.”
- Clogs form when excess oil, dead skin cells, and sticky keratin pile up—not poor hygiene, but a mix of genetics, hormonal shifts, heavy products, or environmental triggers like sweat and pollution.
- Lifestyle choices significantly impact breakouts—smoking doubles your risk, and high-glycemic diets, dairy, heat, and friction from gear all raise the odds of developing comedones.
- Consistent, simple routines beat intense overhauls—use a gentle, non-comedogenic cleanser, oil-free moisturizer, and daily SPF, plus a retinoid or salicylic acid treatment several nights a week.
- Avoid heavy, pore-clogging products and always check for “non-comedogenic” labels; layer thin to thick, and don’t double down on aggressive scrubs or actives.
- Professional help is key when OTC options stall—see a dermatologist if you have scarring, widespread or stubborn comedones, or new red and painful spots after months of effort.
- Comedonal acne is highly manageable with the right mix of habit, product choice, and, if needed, expert support—starting early can stop small bumps from becoming bigger breakouts.
Want more than a surface fix? Dive into the full article for expert-backed strategies, examples, and a no-nonsense approach to building your ideal skin routine.
Introduction
Picture this: You're prepping for a big pitch or video call, only to catch a constellation of tiny bumps dotted across your forehead or jawline—blackheads and whiteheads that seem to pop up no matter how dialed-in your skincare routine is. If you've ever wondered why these stubborn imperfections keep resurfacing, you're in good company among high-performing pros who want clear skin without sacrificing time or tech-driven efficiency.
Here’s a stat worth noting: Over 80% of tech-savvy professionals experience comedonal acne at some point—and while it’s easy to assume more cleansing is the answer, the real culprits are far more complex (and interesting) than you might expect.
So, why should you care right now? Because comedonal acne is the “silent” signal that your skin’s internal processes—much like under-optimized workflows—need a reboot before bigger issues develop. Think of these early-stage blockages as your skin’s version of a subtle error log: easy to overlook, but crucial for avoiding larger, more visible “breakouts” down the line.
You'll discover:
- What actually causes blackheads and whiteheads—and why it’s not about dirt or poor hygiene
- Straightforward strategies to overhaul your routine for faster, more lasting results
- Pro tips to distinguish comedonal acne from other types (so you can target the right fix)
Best of all, this isn’t about adopting a 12-step regimen or chasing miracle cures. It’s about actionable insights and smart habits for smooth, clear skin—even when life gets busy.
Ready to decode what those tiny bumps are really telling you? Let’s get under the surface and see how mastering comedonal acne can give you a proactive edge and set the groundwork for real skin confidence.
The essentials on blackheads and whiteheads—plus the surprising science behind them—are up next.
What Are Blackheads and Whiteheads? The Basics of Comedonal Acne
Comedonal acne is the “early-stage” or non-inflammatory form of acne that tech-minded pros encounter just as often as breakouts with a more dramatic flair.
Unlike those angry, red pimples or swollen cysts, comedonal acne is about clogged pores, not inflammation—think of it as your skin’s notification that something needs tweaking, not a full-blown crisis.
What’s the Real Difference? Blackheads vs. Whiteheads
These common lesions come in two main forms:
- Blackheads (open comedones): Pore stays open, and the plug (oil + dead skin) oxidizes with the air, showing up as a dark spot—like seeing the top of a marker peeking out from a pen holder.
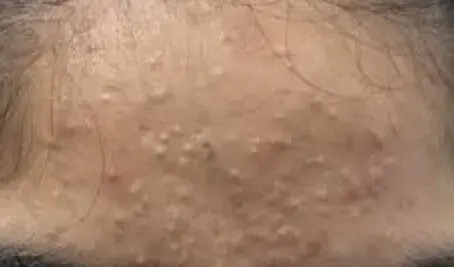
- Whiteheads (closed comedones): Pore opening is sealed by skin, creating a small, slightly raised, white or flesh-toned bump—think of it as a bubble under wallpaper.
Both cause a rough, uneven texture—picture running your hand over the T-zone, cheeks, or jawline and feeling subtle bumps, even if the skin isn’t red.
Setting the Record Straight: Not Dirt, Not Poor Hygiene
It’s a myth that blackheads are just dirt or that whiteheads mean you need to wash your face more.
These plugs form when the mixture of oil, dead skin cells, and sticky keratin gets trapped, not because you skipped a wash.
You’ll often see comedonal acne on:
- Forehead, nose, and chin (T-zone)
- Cheeks and jawline
- Chest and upper back (especially for those who wear gear, collars, or backpacks)
What’s Happening Under the Surface? Picture This
Imagine your pore as a mini factory line—when things run smoothly, the output (oil and skin cells) moves right out the door.
But when the exit gets jammed by excess oil and cells, a line forms at the entrance:
- If there’s no “lid,” oxygen hits the pileup and you get a blackhead
- Add a skin “lid,” and it’s a whitehead—all trapped below the surface
“Think of comedonal acne as traffic congestion—not trash—in your pores.”
One Look, One Lesson
Blackheads and whiteheads are the silent signals your skin sends when the natural system starts to slow down.
Spotting bumps but no redness? You’re looking at comedonal acne—and with the right routine, you can address these early-stage issues before they turn into bigger breakouts.
Your next step? Learn the core causes behind these subtle bumps and see how small changes can make a big impact for your skin’s future.
How Do Blackheads and Whiteheads Form? Core Causes and Risk Factors
Picture this: your skin is like a busy city, where pores are tiny doorways. When these doorways get blocked, blackheads and whiteheads move in. The foundation of comedonal acne is simple—a clogged hair follicle filled with excess sebum (oil), dead skin cells, and sticky keratin.
This trio mixes and plugs up the follicle, trapping material under the skin.
What Really Causes a Follicle to Clog?
Several major contributors drive that clogging process. Think of it as a “perfect storm” brewing:
- Sebum Overproduction: Hormones, especially androgens (like during puberty, menstrual cycles, or with some meds), dial up your skin’s oil factory.
- Abnormal Cell Shedding: For acne-prone skin, dead cells don’t shed cleanly—they clump with oil, creating blockages.
- Comedogenic Products: Look out for “hidden pore-cloggers” like heavy oils, balms, thick sunscreens, and some long-wear makeup.
Even your hair products can be sneaky culprits when they migrate to your face.
Lifestyle and Environmental Triggers to Watch
Lifestyle choices and your environment stack the odds, too. About 80% of people with persistent comedonal acne report exposure to at least one of these:
- Smoking fuels comedonal breakouts (data: risk up to 2x higher in smokers).
- Diet: High-glycemic foods and dairy ramp up sebum and inflammation.
- Heat, humidity, sweat, and pollution increase pore blockages and oil.
- Mechanical and Chemical Irritation: Scrubbing, peel overuse, helmets, masks—anything that rubs or irritates skin can invite more comedones.
A classic gym scenario: workout sweat + occlusive helmet creates a breeding ground for blocked pores.
Genetics: The Built-In Risk Factor
Family history matters—if your parents had comedonal acne, your risk jumps significantly. However, the pattern isn’t always predictable. One sibling might get clear skin, while another battles blackheads.
Current research suggests a “stacking” effect: genetics create the setup, but daily habits and outside factors pull the trigger.
The Big Picture: How It All Adds Up
Imagine your kitchen sink: pour in too much oil, food scraps, and hair, and eventually you get a stubborn clog. Your pores act the same way when oil, skin cells, and debris mix—especially with added irritation or the “wrong” products.
Consistency counts—addressing every contributor above is your best prevention strategy.
Bottom line: Conquering blackheads and whiteheads means managing oil, picking the right products, and limiting outside triggers. The sooner you break the clog cycle, the smoother your skin’s “city streets.”
How Is Comedonal Acne Classified and Where Does It Fit in the Acne Spectrum?
Picture this: you’re reviewing a lineup of acne types, and comedonal acne stands out as the quiet, early-stage contender—no drama, just visible bumps.
Comedonal acne is classified as a non-inflammatory form, meaning you’ll see blackheads and whiteheads without the angry redness of typical pimples.
Most acne can be sorted into two categories:
- Non-inflammatory: blackheads (open comedones), whiteheads (closed comedones)
- Inflammatory: papules, pustules, nodules, cysts (think red, swollen, or painful spots)
80% of teenagers and a surprising number of adults experience comedonal acne, especially along the T-zone, jawline, chest, and back.
When Does Comedonal Acne Overlap with Other Types?
Comedonal acne isn’t always a solo act. In many cases, it shows up alongside or can evolve into more severe acne types.
You might notice:
- Comedones alone: Bumpy texture, especially on forehead and chin
- Combo breakouts: Blackheads/whiteheads with occasional angry red pimples
- Progression: Mild comedonal acne left untreated may “graduate” into inflamed breakouts or cystic lesions
Quick stat: About 60% of patients with moderate to severe acne started with comedonal lesions before developing inflamed spots.
Does Age, Skin Type, or Gender Matter?
Absolutely—patterns can vary widely.
Common trends include:
- Teens and young adults: Comedonal acne is almost a rite of passage
- Oily or combination skin: More prone to visible bumps
- Women in their 20s/30s: Hormonal cycles often drive recurring comedones, especially pre-period
- Men: Higher oil production can mean more stubborn blackheads
If you notice “clusters of tiny bumps” or enlarged pores on your cheeks, you’re seeing classic comedonal patterns.
How Does Comedonal Acne Fit Into the Full Spectrum?
Think of comedonal acne as the foundation layer of the acne pyramid.
It can exist:
- On its own, as persistent but mild bumpy skin
- As a first stage that sometimes leads to papules, pustules, or cysts
Comedones rarely scar if handled properly, but picking or ignoring them can set you up for bigger, longer-lasting breakouts.
Comedonal acne is the “tipping point” on the acne spectrum—a clear sign that your pores need attention before red, inflamed breakouts begin. Recognizing these early bumps puts you in the driver’s seat, giving you time to prevent more severe acne and keep your skin smoother, longer.
Proven Treatments for Blackheads and Whiteheads: What Really Works?
Topical Approaches: The Foundation
If you’re aiming for clear, smooth skin, topical treatments are your front line against blackheads and whiteheads.
The essentials nearly every dermatologist starts with include:
- Topical retinoids (like adapalene or tretinoin) to normalize cell turnover and clear clogged pores—think of these as “decluttering” for your follicles
- Salicylic acid (BHA) in cleansers or leave-on serums, which dives deeply into pores to dissolve oil and debris
- Benzoyl peroxide—especially helpful if you get the occasional inflamed breakout alongside comedones
- Azelaic acid, glycolic acid, or sulfur for mild exfoliation or pigment concerns
Retinoids can take 8–12 weeks to show visible results.
A real-world scenario: Imagine a marketer juggling deadlines, sticking with nightly adapalene and seeing blackheads fade steadily around the three-month mark—it’s about building a habit, not expecting magic overnight.
“Consistency, not intensity, clears comedones—think marathon, not sprint.”
When to Go Prescription or Advanced
Sometimes, what you grab at the drugstore just isn’t enough.
Dermatologists step in when:
- Comedonal acne won’t budge after months of proper OTC care (picture: cheeks dotted with stubborn whiteheads despite everything)
- You need stronger retinoids, or short courses of oral isotretinoin for severe or scarring-prone cases
- Bonus insight: Oral and topical prescriptions are matched to your skin’s sensitivity and unique response
Antibiotics are rarely used for pure comedonal acne—only if things get red and angry, and even then, antibiotic-resistance is a real concern in 2024.
“You don’t have to ‘tough it out’—tech-savvy routines + expert help can banish even persistent comedones.”
In-Office & Professional Help
Some comedones refuse to leave—enter the pros.
In-office options might include:
- Comedone extraction: fast, satisfying, and way safer in expert hands than at home
- Chemical peels (salicylic/glycolic acid) or microdermabrasion for an all-over texture boost
- Expect costs from $75–$200 per session, usually spaced 2–4 weeks apart
A dermatologist will recommend these for dense or “closed” comedones, or when your routine alone can’t keep up.
You’ll want to skip DIY popping—improper technique causes scarring, and one session with a pro can do more than months of mistakes.
Picture this: crisp, clear skin after a series of pro peels, without battling red marks or scabs for weeks.
Effective comedonal acne treatment is built on proven active ingredients, realistic timelines, and the occasional pro assist. Stick with science-backed routines and don’t hesitate to ask for expert help—your future self (and skin) will thank you.
Building a Routine: Daily Practices for Clearer, Clog-Free Skin
Skincare Habits for Prevention and Management
The fastest path to clearer skin? Consistency beats perfection for managing blackheads and whiteheads.
Picture this: You wake up, your face feels smoother, and you’re not stressing about bumps. Here’s a simple, effective daily routine:
- Morning:
- Cleanse with a gentle, non-comedogenic cleanser (skip the harsh scrubs).
- Apply a lightweight, oil-free moisturizer.
- Finish with a broad-spectrum SPF 30+ sunscreen labeled “won’t clog pores.”
- Evening:
- Double cleanse at night—first with a gentle makeup remover or micellar water, then with your regular cleanser.
- Add a targeted treatment (like a retinoid or salicylic acid) every other night.
- Moisturize to maintain your barrier.
Tick this routine off daily, and you’re already ahead of most people.
Product Choices and Application Tips
Ever stood in the skincare aisle squinting at labels? Here’s what matters most for acne-prone skin:
- Look for “non-comedogenic” and “oil-free” on all products.
- Avoid these red-flag ingredients:
- Coconut oil
- Isopropyl myristate
- Thick balms or butters
- Optional extras:
- Niacinamide serum for oil balance and barrier repair
- Clay or charcoal masks once a week for oil control (not daily!)
Pro tip: Layer thin to thick—start with treatments, end with moisturizer and sunscreen.
Two common mistakes? Using too many actives at once, or over-cleansing (twice a day is plenty). “Go slow so you can glow” is truly skincare gold.
Lifestyle Factors
Your daily choices matter as much as your products—sometimes more.
- Aim for a lower-glycemic diet (think: less white bread, more veggies).
- Consider cutting back on dairy if breakouts are stubborn.
- Never pick or squeeze—that quick fix often leads to scars or more pimples.
- After sweating or working out, cleanse your skin and swap into clean clothes ASAP.
- If you smoke, quitting can seriously up your skin’s game—a major cause of comedonal acne.
- Avoid friction from hats, masks, or gear on breakout-prone areas.
Small adjustments here can unlock big wins for skin—you’ll literally see the difference in weeks, not years.
The best routines are realistic, repeatable, and gentle. If you stick with this approach, you’re setting up your skin (and your sanity) for long-term success—no 10-step routine required.
When to Call in the Pros: Signs You Need Professional Help
Knowing when to DIY and when to bring in the experts is crucial for conquering comedonal acne.
If you spot any of these signs, it’s time to call a dermatologist:
- Scarring: New pitted marks or dark spots won’t fade
- Widespread comedones: Large areas covered in blackheads or whiteheads
- Stubborn acne: No major improvement after 2–3 months of consistent over-the-counter (OTC) care
- Red, painful, or cystic lesions: Signs you have more than mild comedones
Picture standing in front of your bathroom mirror—months have gone by, yet your skin still feels bumpy, with new clogs appearing every week.
“If you feel like you’ve tried everything and your skin is still fighting back, it’s not a failure—it’s just time for backup.”
When Your Routine Isn’t Enough
Sometimes, sensitive skin, reactions to retinoids or acids, or managing a complex product lineup can make things overwhelming.
If you’re not sure why things aren’t working or you’re dealing with:
- Unusual side effects (stinging, worsening breakouts, extreme dryness)
- Difficulty sticking to routines because of confusion or frustration
- Family history of severe acne or scarring
That’s a sign you need a pro’s guidance.
What a Dermatologist Offers That Drugstore Shelves Can’t
Dermatologists bring out the “big guns”—from prescription-strength retinoids to short-term oral treatments and highly tailored plans.
Here’s what you might get:
- Custom prescription options (stronger topicals, oral medication, or combination therapy)
- Professional procedures: like comedone extraction, chemical peels, or microdermabrasion—costs can range from $80 to $300+ per session
- Safety monitoring for complex regimens (especially if your skin’s sensitive or you react to actives)
You get both a plan and a coach—empowerment, never defeat.
“Dermatology isn’t just for the ‘worst cases’—it’s a smart investment in your skin’s future when at-home tools aren’t getting results.”
Make the Most of Pro Support
Think of reaching out as calling in an expert for your business—sometimes the outside perspective and upgraded tools are what unlock real progress.
If you're noticing scarring, spreading comedones, or zero change after months of good habits, take action sooner rather than later. The right help now can save years of frustration (and future regrets over scars). Empowerment starts with taking your skin seriously.
Conclusion
Comedonal acne doesn't have to run your day—or your confidence. The real power lies in understanding the mechanics behind blackheads and whiteheads, then applying smart, consistent strategies that fit a tech-savvy, solution-oriented lifestyle.
When you focus on practical routines and intentional choices, you're not just reacting to bumps—you're proactively optimizing your skin’s future.
Here’s what makes the biggest impact:
- Choose truly non-comedogenic products—review ingredient lists, not just labels.
- Build a sustainable daily routine—gentle cleansing, targeted treatments, and SPF are key.
- Tweak your habits—right after sweating, cleanse and change clothes to minimize pore congestion.
- Address underlying factors—consider reducing high-glycemic foods, monitoring dairy, and managing stress.
- Know when to level up—if progress stalls, dermatology support can unlock expert solutions fast.
Ready to take action?
- Audit your current skincare products for hidden pore-cloggers and swap where needed.
- Set a 60-day reminder to track concrete changes from your new routine.
- Schedule a consult with a dermatologist if you spot scarring, increased breakouts, or frustration mounting.
- Share your progress—compare before/after steps, and empower others in your network to start smart.
Your skin is an investment—every small, consistent step is a data point in your success story.
Notice the signals, optimize your routine, and act early. The most effective long-term results come from taking charge before small issues escalate.
Clearer, smoother skin isn’t just possible—it’s within your reach, one informed choice at a time.
“The best breakthroughs happen when you treat your skin like you run your business: analyze, adapt, and never settle for less than progress.”