Key Takeaways
Understanding whether you’re dealing with inflammatory or non-inflammatory acne instantly transforms your treatment approach—and can seriously speed up your results. Here’s what tech-savvy professionals and ambitious creators need to know to level up their skin strategy without wasting time (or money) on the wrong methods.
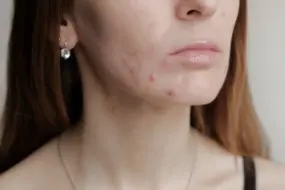
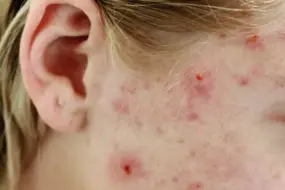
- Know your acne type first—spot the difference by identifying non-inflammatory acne as painless bumps (blackheads/whiteheads) versus inflammatory acne as red, swollen, or tender lesions.
- Both types start with clogged pores, but inflammation kicks in when bacteria trigger your immune response, leading to more visible redness, swelling, and pain.
- Non-inflammatory acne rarely scars, so reach for pore-uncloggers like retinoids and salicylic acid—most options are over-the-counter and preventative.
- Inflammatory acne demands fast action—target with anti-inflammatories (benzoyl peroxide, antibiotics) or see a dermatologist for deep, painful lesions to minimize scarring risk.
- Misclassifying your acne delays results—studies show a tailored “type-first” routine can reduce severity by up to 60% and halve scarring risk, helping you stay camera-ready.
- Visual and sensory cues matter—if you feel pain, see swelling, or notice color changes (redness, purple), shift your routine and escalate care as needed.
- Proactive tracking pays off—use digital tools or weekly photo logs to map trends and triggers, making it easier to catch escalation or link flare-ups to specific habits.
Spotting the true type of acne you have is the smartest, fastest route to clear skin—and a confident, professional presence. Dive into the full article to get expert strategies and examples that fit your workflow.
Introduction
Ever stared at your bathroom mirror, wondering why one pimple is a quiet bump while another cries out with redness and pain? You’re definitely not alone—and the answer lies in a critical difference: not all acne is created equal.
Here’s a shocker: Roughly 85% of people experience acne at some point, but did you know that identifying whether your breakouts are inflammatory or non-inflammatory can cut your treatment time in half?
For tech-driven pros juggling deadlines (and maybe a Zoom call you wish had a beauty filter), getting the type right means:
- Quicker relief from visible breakouts (hello, confidence boost)
- Smarter, more targeted use of topicals and routines (less money wasted)
- A lower risk of scars that outlast your latest project
Think of it as debugging your skin: when you spot the unique “code” behind each breakout, you can ditch guesswork and apply real solutions—fast.
But here’s where most advice fails: it treats every breakout the same, missing the fact that a blackhead and a cyst are totally different scenarios. Knowing the distinction between these subtypes helps you separate cosmetic annoyances from urgent red flags—and ensures you’re not just treating, but actually preventing the next flare-up.
Quick takeaway: When you can tell whether you’re facing a “silent traffic jam” (non-inflammatory) or a “full-blown street brawl” (inflammatory), you’ll skip the endless product roulette and finally give your skin what it needs.
Get ready to decode acne like a pro. Up next, we’ll break down exactly what sets these two types apart—and show you how to spot the telltale signs, so you can intervene with confidence and precision.
Understanding the Basics: What Are Inflammatory and Non-Inflammatory Acne?
Trying to make sense of your breakouts? You're not alone. The most important split in the acne world comes down to inflammatory versus non-inflammatory acne—and knowing the difference can totally change your treatment strategy.
Both types of acne start the same way: with a clogged pore, known as a microcomedo. Picture this: dead skin cells, extra oil (sebum), and sometimes bacteria getting packed inside a tiny skin “traffic jam.”
But from here, those blockages can go two directions:
- If things stay quiet, you get non-inflammatory acne—think blackheads and whiteheads, barely noticeable beyond a bumpy texture.
- If your defense system kicks in, you’ll end up with inflammatory acne—red, swollen, and often painful.
Red Alert vs. Silent Jam: The Core Difference
Let’s use an analogy. Non-inflammatory acne is like a minor traffic jam—annoying but calm under the skin.
Inflammatory acne is a blaring alarm triggered by outside invaders—your body reacts, causing redness, swelling, and tenderness.
The difference comes down to:
- Inflammation (redness, swelling, pain)
- Type of lesion (bump only vs. bump plus angry skin)
- Risk of scarring (much higher with inflammation)
If your pimples hurt, look red, or swell up, that’s a sign you’re dealing with something deeper.
How Acne Forms: The Shared Starting Point
Both types begin with:
- Excess sebum (oil) production
- Build-up of dead skin cells
- Bacterial presence (especially Cutibacterium acnes)
The sequence usually goes like this:
- Pore clogs (microcomedo)
- Turns into a blackhead or whitehead (non-inflammatory), or
- Bacteria trigger your immune response, turning it into a red, swollen lesion (inflammatory)
Here’s the key visual:
- Non-inflammatory acne = bumps, but no redness
- Inflammatory acne = bumps + red, swollen, sometimes pus-filled spots
Why Classification Changes Everything
Understanding which type you have guides:
- Which products to reach for: unclogging agents vs. anti-inflammatories
- When to escalate: OTC vs. seeing a dermatologist
- Chances of scarring: inflammatory types need faster, stronger action
Quotable tip: “Think of non-inflammatory acne as clogged highways, and inflammatory acne as road rage—same starting point, but a very different journey for your skin.”
So if you're seeing only tiny bumps, it's not just cosmetic—catching them early helps stop bigger, redder problems down the line. If pain, redness, or swelling show up, it's time to act fast and maybe bring in professional backup.
Key takeaway: Knowing which kind of acne you have sets you on the right treatment road, lowers frustration, and can seriously cut your risk of long-term skin issues.
Non-Inflammatory Acne: Features, Subtypes, and What to Look For
Non-inflammatory acne, or comedonal acne, is the “quiet” side of breakouts—it’s all about clogged pores that aren’t red, swollen, or painful.
Picture this: you see small bumps on your face, but nothing looks angry or feels sore. These are mostly cosmetic concerns that rarely scar, especially if you leave them alone (please, hands off!).
If you catch these early, you can often prevent your skin from sliding into more severe, inflamed territory.
The Two Main Players: Blackheads and Whiteheads
Non-inflammatory acne comes in two flavors:
- Blackheads (open comedones):
- Look like tiny dark dots or specks—think miniature “freckles” with a gritty feel.
- The dark color isn’t dirt or poor hygiene; it’s actually oxidized oil and dead skin cells.
- Whiteheads (closed comedones):
- Appear as small, firm, skin-colored or slightly white bumps.
- Usually not red, not tender, and can be felt more than seen, especially in good lighting.
You’ll most often spot these on the forehead, nose, chin, and cheeks—classic T-zone territory, but shoulders and chest can get them too.
Recognizing the Symptoms
Non-inflammatory acne almost never hurts.
Classic symptoms include:
- No pain or tenderness
- Little to no swelling
- Minimal redness or warmth
Most people notice these as subtle texture—the kind where you run your hand over your skin and feel tiny, sandpaper-like dots.
“Ever scanned your face in a magnifying mirror and wondered about those sprinkled bumps? Chances are, you’re looking at non-inflammatory acne.”
Risks, Severity, and Progression Potential
Non-inflammatory acne is usually mild and persistent, but it can creep up in severity if left unchecked.
Watch for common progression triggers like:
- Frequent skin touching or picking
- Inconsistent cleansing or heavy, pore-clogging products
- Hormonal shifts (think teenagers or stress)
Hyperpigmentation or marks are rare—unless you scratch, squeeze, or have chronic lesions that linger.
Here’s an eye-opener: “Silent” comedonal acne can still dent confidence, especially if you feel like you’re the only one who ever notices it.
If you spot early blackheads or whiteheads, acting quickly with gentle, proven solutions can keep things under control—think prevention, not just reaction. Not all acne is “angry”—but all acne deserves the right game plan.
Inflammatory Acne: Understanding the Red, Swollen, and Painful Side
Inflammatory acne is the red-alert version of your everyday breakout—painful, often swollen, and ready to hijack your confidence.
What sets it apart? Inflammatory lesions go beyond simple clogged pores, as your immune system launches a response to bacteria trapped inside, triggering redness, swelling, and tenderness.
Think of it like this: non-inflammatory acne is a quiet traffic jam, while inflammatory acne is when sirens are blaring and the street’s blocked off.
Why does this matter? These types are more likely to scar and almost always require faster, sometimes medical, intervention. That’s why recognizing them early changes everything for long-term skin health.
Key Lesion Types: From Papules to Nodules and Cysts
You’ll spot inflammatory acne by these classic offenders:
- Papules – Small, red, tender bumps with no visible pus
- Pustules – Red bumps topped with a white or yellow center, pus-filled
- Nodules – Large, firm, deep lumps that hurt when touched
- Cysts/Pseudocysts – Deeper, softer, often fluid-filled; can merge with other lesions
Quick Comparison Chart:
Every type steps up the likelihood of long-term marks, especially cysts and nodules, so early action is key.
Symptoms and Visual Cues
Wondering if it’s inflammatory? Look for redness, swelling, warmth, and pain—the kind of spot that makes you say “ouch” when you wash your face.
Typical hotspots include:
- Jawline
- Cheeks
- Chest
- Upper back
When to escalate care:
- Lesions persist more than a few weeks
- Pain disrupts daily life or sleep
- Scars or dark spots start to form
Picture this: a large, painful bump under your skin that doesn’t budge—classic nodule territory.
These breakouts aren’t just physical; they seriously affect how confident you feel stepping into a meeting or joining a video call.
Underlying Causes & Exacerbating Factors
The culprit behind inflammation? Cutibacterium acnes—a bacteria that thrives in blocked pores and triggers your immune system’s “attack mode.”
But why you?
- Hormones: Surges during puberty, periods, or stress can turbocharge oil glands
- Stress: Messes with skin’s defenses
- Humidity & Diet: Oily climates and high-glycemic foods can fuel flare-ups
- Picking or friction: Break down skin barriers and invite infection
- Genetics & Environment: If your parents had it, you’re likely a candidate
Imagine battling a nasty breakout right before an important presentation—your stress could actually make those pimples angrier.
If you spot red, sore, or unusually persistent bumps, it’s time to take action—these require targeted treatments and sometimes professional help to avoid long-term scars. Remember: fast recognition and intervention can be the difference between a quick fix and years of regret.
Why This Classification Matters: Implications for Treatment and Outcomes
Knowing whether your acne is inflammatory or non-inflammatory isn’t just a technical detail—it directly shapes how fast you’ll see results, which products actually work, and how likely you are to deal with scarring or pigmentation down the line.
Picture this: Trying to treat red, swollen cysts with the same routine you’d use for little blackheads is like using a wrench to fix a software bug—wrong tool, slow results, major frustration.
If you get the type wrong:
- Treatment can stall for weeks or months
- You may increase your risk of permanent scarring
- Over-the-counter fixes might waste your time—and money
This “know-your-acne-type” approach pays off: According to recent studies, early targeted treatment can reduce acne severity by up to 60% and cut future scarring risk by half.
High-Level Treatment Frameworks
Let’s break it down by category—because your face isn’t one-size-fits-all.
- Non-Inflammatory Acne (Whiteheads/Blackheads):
- Focus on unclogging pores and keeping cell turnover steady.
- Crowd favorites include topical retinoids, salicylic acid, and gentle chemical exfoliants.
- Most options are over-the-counter and easy to add to your nightly routine.
- Inflammatory Acne (Papules, Pustules, Nodules, Cysts):
- Attack bacteria and dial down inflammation with benzoyl peroxide, antibiotics, or prescription retinoids.
- Hormonal therapy and oral isotretinoin are game changers for severe cases.
- The sooner you address inflammation, the lower your risk of lasting marks.
- See a dermatologist if you notice deep, painful lumps or rapid worsening.
Combo skin woes? Many need a blend of both strategies—think “layering armor,” not just picking one side.
Cheat sheet:
- Mild, painless bumps: stick with pore-uncloggers.
- Red, painful, or swelling: layer on anti-inflammatory tools, and don’t wait to call your dermatologist.
Scarring, Pigment Changes, and Long-Term Skin Health
Here’s what really matters: non-inflammatory acne is unlikely to scar, while nodules and cysts can leave marks that last for years—or forever.
Your action plan to win the long game:
- For comedones: Hands off!—no picking.
- For inflamed lesions: Start proven treatment ASAP to prevent damage to deeper skin.
- Consider adding a sunscreen and vitamin C serum to prevent hyperpigmentation.
If you’ve ever seen a breakout fade but a dark spot remains, that’s post-inflammatory pigmentation—treat early, fade faster.
Getting your acne classification right isn’t about labels—it’s about faster results, fewer scars, and smarter routines. Think of it as customizing your workflow: once you know the “problem type,” you can deploy the exact tools that actually get it fixed.
Mapping Your Acne: Visual and Symptomatic Self-Assessment
Wondering if your acne is inflammatory, non-inflammatory, or a bit of both? An easy self-assessment can reveal the story your skin is telling—no microscope or medical degree needed.
The key is knowing what to look for, where it appears, and how it feels. Most breakouts offer clear visual and sensory signals that can guide your next steps—whether that’s tweaking your routine or booking a dermatologist appointment.
Step-by-Step: How to Map Your Breakouts
Start by facing the mirror (bonus points if you turn on that super-bright selfie light). Walk through this checklist:
- Examine lesions closely:
- Are most bumps skin-colored or dark-topped (think blackheads/whiteheads)?
- Or are they red, swollen, or tender (think pimples, cysts)?
- Assess for pain and swelling:
- Do you feel pain or tenderness?
- Or are the bumps mostly painless to touch?
- Spot color and pigmentation:
- Is there no redness, or do spots have pink, red, or even purple tones?
- Do marks linger after healing (dark spots or scarring)?
- Log the locations:
- Are breakouts clustered on the forehead, nose, or chin (comedonal common zones)?
- Or do you have deeper breakouts on the jawline, back, or chest (inflammatory hot spots)?
Quick-Reference Chart: What Does Your Acne Say?
Trends & Tools for Proactive Skin Tracking
Digital apps make it simple to track flare-ups over time. Snap photos weekly, jot down triggers, or set reminders to monitor skincare changes.
- Use photo logs:
- Track how lesions change or if new types emerge.
- Note timing:
- Does your acne flare with stress, cycle, or certain foods?
Pro tip: “If new breakouts are rapidly increasing in redness, size, or pain—or you notice deep nodules—it’s time to consult a pro.”
A quick, honest mapping session can help you spot patterns, catch escalation early, and choose treatments that match your acne’s true type. Treating what you actually have—rather than guessing—makes all the difference for faster relief and better long-term results.
Conclusion
Decoding whether you’re facing inflammatory or non-inflammatory acne can be a game-changer for your skin—and your confidence. When you understand the true nature of your breakouts, you unlock a smarter, more effective path forward that’s tailored to your actual needs.
You don’t have to gamble or second-guess your routine. By recognizing the signals your skin sends, you can finally move from frustration to focused action—with treatments that genuinely work and a strategy designed for real results.
Key Takeaways:
- Identify your breakout type before choosing products—non-inflammatory and inflammatory acne demand targeted solutions.
- Track symptoms and patterns (pain, redness, swelling, location) for the clearest roadmap to what your skin truly needs.
- Avoid picking or squeezing—it raises your risk of scarring, especially with inflammatory lesions.
- Escalate to professional care if you notice persistent pain, swelling, or scarring risk—timing here really matters.
- Harness digital tools or photo logs to keep a close eye on your skin’s progress and triggers.
Immediate Next Steps:
- Map your current acne in the mirror, noting type, color, and pain level.
- Update your skincare routine to match what you’ve learned: add proven ingredients, or swap out what’s not helping.
- Set a check-in reminder—review your skin’s response weekly and tweak your plan.
- Reach out to a dermatologist if severe or fast-moving inflammation appears; early intervention prevents lifelong marks.
Your skin deserves a treatment plan as unique and dynamic as you are. Take the first step today—tune in, act with intention, and watch your skin start to tell a brighter story.
Because treating acne isn’t just about clearer skin—it’s about showing up every day with more confidence and control. Ready to hit reset? Start with the knowledge you own now, and transform frustration into real momentum.
“Your acne isn’t the headline of your story. Knowing what type you have? That’s your power move.”