Key Takeaways
Noticing changes in your toenails can seem minor, but knowing when to see a doctor for toe fungus is crucial for your long-term foot health—and peace of mind. Scan these expert-backed insights to quickly understand when DIY care stops and professional help becomes a must.
- Recognize toe fungus early by watching for persistent discoloration, thickening, or crumbling nails—acting fast prevents bigger problems down the line.
- See a doctor if symptoms last more than 2–4 weeks despite home remedies, especially if you experience pain, spreading, odor, or difficulty trimming your nail.
- Don’t wait if you’re high-risk—people with diabetes, weakened immunity, or poor circulation are more likely to develop serious complications from even minor infections.
- Leave recurring or worsening infections to specialists; trying to out-stubborn toe fungus increases your risk for permanent nail damage and secondary infections.
- Specialist visits provide accurate diagnosis through lab testing, saving you from months of ineffective treatments and speeding up your recovery plan.
- Early intervention means easier, shorter treatment—over 70% of patients improve quickly when seeking medical help within the first 6 months of symptoms.
- Prevention matters post-treatment: Keep feet clean, dry, and protected—since 20–25% of cases can recur without strong self-care habits and regular checks.
Prioritizing your foot health means knowing when to ask for expert help—review our full article to protect your comfort, avoid costly delays, and keep your step strong at any pace.
Introduction
You’re late for your morning meeting, grab your shoes, and there it is—a thick, yellow nail looking back at you. Sound familiar? Nearly 1 in 7 people will wrestle with toe fungus at some point, and it often starts as just an annoying spot before spiraling into something you can’t ignore.
For tech-driven professionals like you, minor health hassles can quickly snowball into major distractions. You might brush off a discolored toenail as a small inconvenience—until it starts catching on socks, making shoes uncomfortable, or refusing to clear up no matter which spray or lotion you try.
Here’s the thing: more than 70% of mild infections don’t clear up with home remedies alone. When you’re optimizing workflows or automating your marketing stack, the last thing you need is a health issue sabotaging your momentum, especially when fast intervention could make all the difference.
So…how do you know if it’s time to call in a pro?
This guide delivers actionable answers at the speed you need.
You’ll discover:
- Clear warning signs that mean it’s smart (and cost-effective) to see a doctor
- Risks and red flags you should never ignore, especially for those juggling tight deadlines or chronic conditions
- Real-world scenarios that make the blurry line between DIY and professional care easy to spot
- Tips for prepping smarter for your appointment, so no time (or energy) is wasted
Think of this as the decision-making cheat sheet for toe fungus—practical, concise, and built for your on-the-go lifestyle.
Ready to gain back control—and kick “nail shame” out of your weekly routine? Up next, we’ll tackle what toe fungus really is and how it can quietly hijack your day if left unchecked.
Understanding Toe Fungus and Its Impact
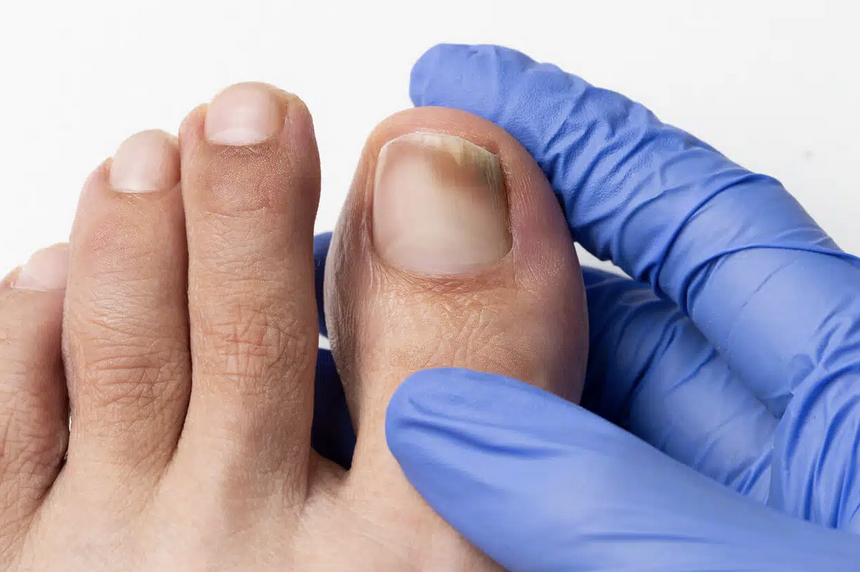
Toe fungus, known medically as onychomycosis, is a common nail infection caused by fungi that thrive in warm, damp environments—picture locker rooms, sweaty socks, or shared showers.
You might notice it starting as a yellow or white spot under the toenail, gradually spreading and thickening the nail.
Left unchecked, it can cause nails to crumble, distort, or separate from the nail bed—a detail that’s glaringly obvious if your sock catches on a jagged edge.
How Common Is Toe Fungus?
It’s more common than most think: up to 14% of the population will deal with toe fungus at some point.
Adults over 60 are especially at risk, but anyone frequenting gyms, pools, or communal spaces can pick it up.
If you’re juggling deadlines and dashing between meetings, a discolored or brittle nail can seem minor—until it’s not.
Why Recognition (and Fast Action) Matters
Recognizing early signs is essential because untreated toe fungus can:
- Lead to permanent nail damage
- Cause secondary infections, particularly if you have diabetes or a weakened immune system
- Spread to other nails or even to others nearby
According to recent dermatology data, only about 15–30% of mild cases resolve with home remedies—which means most need more than basic care.
Mild Versus Medically Needy: What’s the Difference?
Some cases are mild—think:
- A faint spot that hasn’t changed for weeks
- No pain, no odor, no thickening or spreading
But if you notice:
- Persistent color changes or thickening lasting longer than 2–4 weeks
- Increasing pain, odor, or difficulty trimming the nail
—it’s time to consider expert help so you don’t risk long-term complications.
Spotting Early Warning Signs in Real Life
Imagine you’re slipping on loafers for work and notice a nail that’s yellow, thicker, and snagging your socks every morning.
Or your weekend run ends with soreness around a darkened nail that's starting to lift.
These are not just annoyances—they’re classic signals your body wants help.
Acting early can save time, money, and stress.
If you spot nail changes that won’t disappear or start interfering with daily life, the smart move is to put a podiatrist or dermatologist on speed dial.
Quick recognition means you’re not risking a minor issue snowballing into something more severe—and that’s one less thing to worry about during your busiest weeks.
Key Signs and Symptoms Requiring Professional Attention
When it comes to toe fungus, your smart move is knowing when it’s time to call in a pro. Some symptoms are your body’s way of waving a big red flag—don’t ignore them.
If you spot any of these, it’s your green light to book an appointment:
Fast-Track the Decision: “Red Flag” Checklist
- Persistent discoloration (yellow, brown, black, or white spots/streaks that don’t budge)
- Nail thickening, crumbling, or strange shapes (nails get harder to trim, chunkier, or just look wrong)
- Pain, soreness, or discomfort that makes walking or wearing shoes annoying—picture this: every step feels like a pebble in your shoe, all because of one nail
- Lifting or separation of the nail from its bed (onycholysis)
- Bad odor that sticks around despite your best hygiene—think: “I just showered, but my toe still smells off.”
- Swelling, redness, or bleeding near the nail, especially if it’s tender or oozing
- Spreading infection beyond one nail, to the skin, or just not getting better after 2-4 weeks of over-the-counter care
Real-Life Scenarios and Warning Signals
You notice your big toenail is turning yellow and getting crumbly—now your shoe feels tight, and every step pinches. Or maybe that white spot you brushed off last month has turned into a thick, bumpy monster. If symptoms drag on past a few weeks, or they’re getting worse, home remedies probably won’t cut it.
Look for patterns: discoloration, pain, or weird nail growth that persists or spreads is a cue for action.
When to Move from DIY to DME (Doctor, My Expert)
- Changes hang around or get worse after 2-4 weeks
- You have pain that messes with your daily routine
- The infection is marching over more nails or skin
If your symptoms tick any of these boxes, don’t wait—it’s the difference between a quick fix and a long, expensive recovery.
Your actionable takeaway: If your toe fungus refuses to improve, causes pain, or spreads—especially after a month—skip home care and let a specialist step in. That’s the easiest way to protect your nails, comfort, and peace of mind.
High-Risk Populations and Situations: When to Seek Care Immediately
If you've got toe fungus and fit into certain groups, it’s not just a cosmetic issue—it can quickly turn into something far more serious.
Act fast if you’re in one of these high-risk brackets:
- People with diabetes: Poor circulation and reduced nerve function can mean a tiny infection becomes a bigger health problem before you even feel pain.
- Immunocompromised individuals: Whether it’s because of medications, chemotherapy, HIV, or organ transplants, your body's defenses are already working overtime.
- Older adults or anyone with poor peripheral circulation: Age or vascular issues slow healing and increase risk for complications.
Watch for Situational Triggers
Some situations should have you dialing your podiatrist’s office—no hesitations.
- Infections that keep coming back or don’t budge after a few weeks of OTC remedies: Persistent issues often need prescription-strength solutions.
- Not sure if it’s fungus or something else? Psoriasis, injury, or eczema can all look similar—misdiagnosis can delay the right treatment.
- Trouble walking, standing, or wearing shoes: If symptoms are interfering with daily life, it’s not “just a nail problem”—it’s an urgent quality-of-life issue.
Don't Risk Delaying Medical Care
Delaying professional treatment in these scenarios can lead to:
- Permanent nail damage (think thick, misshapen, or lost nails)
- Secondary infections—sometimes spreading to bone or deep tissue
- Systemic spread, especially for people with weak immune systems
- Loss of mobility or prolonged pain that limits work and activity
Picture this: An elderly patient with diabetes develops toe fungus but waits six months to see a doctor—what started as a small yellow patch ends up with a bacterial infection requiring months of antibiotics and partial nail removal. No one wants to be that statistic.
High-Stakes Cases: Outcomes and Quick Data
- Studies show that people with diabetes are twice as likely to experience serious complications from untreated toe fungus than those without.
- Immunocompromised patients face up to a 30% higher risk of infection spreading beyond the nail if not treated early.
If you or someone you know checks any of these boxes, don’t wait. The most powerful way to prevent long-term damage is to get prompt professional care—sometimes, one quick visit is all it takes to tip the odds in your favor.
The Diagnostic Journey: What to Expect When You See a Specialist
Booking a visit with a podiatrist or dermatologist is your next logical step if toe fungus isn’t improving. Picture this: you walk into the exam room, and instead of guessing, you get answers backed by science and years of clinical experience.
What Happens During Your Appointment
A typical specialist visit for toe fungus includes three focused stages:
- Detailed history: Expect questions like “When did you first notice nail changes?” or “Have you tried over-the-counter treatments yet?”
- Physical exam: The doctor will examine your feet and nails closely, noting color, thickness, and any signs of spreading.
- Diagnostic lab testing: They may take a nail clipping, scraping, or swab to send for advanced analysis, such as microscopy, culture, or PCR. These tests can identify fungus types—or spot another issue masquerading as toe fungus.
Lab Testing: Why It Matters
Lab results are the gold standard. They:
- Confirm a fungal infection (not psoriasis, trauma, or bacteria)
- Reveal the best match for prescription treatments
- Reduce wasted time on the wrong remedies
It’s not just a nail problem. Accurate diagnosis is your shortcut to faster cure rates—some studies show up to 80% accuracy improvement over visual checks alone.
What About Insurance and Documentation?
Specialists use ICD-10 codes for toe fungus—like B35.1 (onychomycosis)—for transparent communication with insurance providers. This helps streamline billing, minimize claim denials, and keeps records accurate. (Curious? Check our sub-page for the latest ICD-10 list and tips.)
How Diagnosis Shapes Your Next Moves
With confirmed results, your doctor will:
- Outline options: topical meds, oral antifungals, laser treatment, or, rarely, nail removal
- Set realistic expectations: how long each treatment may take, and what side effects to watch for
- Share early prevention tactics to stop fungus from coming back or spreading to others
Memorable Moments & Immediate Takeaways
Picture the confidence in finally knowing what’s beneath your discolored nail. “Most people feel relieved just having a clear plan—no more guesswork.”
Lab confirmation protects you from months of ineffective DIY treatments. Precise diagnosis means a tailored attack plan and faster results.
When you know what to expect from a specialist, you’re not just addressing symptoms—you’re taking actual control of your foot health. Armed with the right diagnosis, you can pivot to the smartest, most effective next steps right away.
How Early Intervention Shapes Outcomes
Why Acting Fast Matters
When it comes to toe fungus, time isn’t on your side.
Seeing a doctor early can boost your chance of a full recovery—over 70% of patients see improvement when treated within the first 6 months of symptoms.
Waiting it out? That typically means a tougher road and higher costs down the line.
“Acting fast on toe fungus is like catching a leak before it floods your basement.”
Advantages of Prompt Treatment
The benefits of getting ahead of your infection are clear.
Patients who seek help at early symptom onset are far more likely to:
- Experience shorter treatment times (often 3-6 months vs. 12+ months for advanced cases)
- Prevent permanent nail damage before it starts
- Avoid secondary infections that can affect other toes, skin, or even become systemic
- Skip aggressive steps like total nail removal or long-term oral medication
Picture this: treating a single discolored toenail now, instead of losing half your nails to unchecked infection a year later.
What Happens If You Wait?
Procrastination rarely works in your favor here.
Delaying care often means:
- Longer, costlier treatments (think $500+ in specialist visits and prescriptions)
- Greater risk of spreading fungi to every sock, shoe, and family member
- Higher chance of permanent nail loss or recurring, chronic infection
About 30% of untreated cases see complications that require surgical removal or months of oral antifungals—ouch.
Data, Trends, and Myths
Current trends show more people waiting, hoping mild infections will “just go away.”
But studies consistently debunk this: fungal nail infections don’t resolve on their own once established.
“Waiting it out” is more likely to mean waiting for it to get worse.
Expert tip: The quicker you treat, the faster and cheaper your recovery.
Takeaway
Early action is the real shortcut when it comes to toe fungus.
Book your appointment at the first sign of trouble—you’ll save time, skip painful interventions, and stay a step ahead of chronic issues.
Find out how you can create a proactive care plan on our detailed sub-pages and start protecting your feet, fast.
Next Steps: Navigating Care, Treatment, and Prevention
Booking an appointment is your first step—get on your podiatrist’s calendar as soon as you notice persistent symptoms or risk factors.
Prep for your visit by making a quick list:
- Track symptoms: When did they start, what has changed?
- Note any home treatments you’ve tried and for how long.
- Jot down daily impact: Is it hard to walk, or do shoes feel uncomfortable?
“Picture this: You slide off your socks, spot yellow streaks, and realize a podiatrist appointment is the logical next move—don’t wait until it interferes with your run or standing at your desk.”
Exploring Treatment Options: What to Expect
Effective treatments depend on the type and severity of your infection—it's not one-size-fits-all.
Here's what your provider may recommend:
- Topical antifungals: Creams, solutions, or lacquers for mild cases; usually daily application for 6-12 months.
- Oral medications: Prescription pills (like terbinafine or itraconazole) for persistent infections; typical course lasts 3-4 months, with cure rates around 60-80%.
- Advanced therapies: Laser treatment, photodynamic therapy, or, if needed, complete nail removal for severe or unresponsive cases.
Be ready for gradual change. “Expect slow progress—clearing a toenail fungus can take months, not weeks.”
Beyond Treatment: Preventing Future Infections
Post-treatment, prevention is your forever priority.
Here’s your prevention checklist:
- Keep feet clean and dry—change socks daily, rotate shoes, and don’t let sweat linger.
- Use antifungal sprays or powders in shoes, especially if you frequent gyms or pools.
- Disinfect nail tools and avoid sharing them.
- Choose breathable footwear and skip walking barefoot in shared areas.
Remember: Even after a successful cure, 20-25% of patients experience recurrence—staying vigilant is key.
Building Smarter Health Habits
Real-world scenario: You’ve tackled your first infection, but what’s next?
Schedule regular foot check-ins. Upgrade to moisture-wicking socks. Remind yourself with smart-device alerts to air out shoes.
Don’t stop at relief—visit our resources on advanced therapy options, self-care routines, and long-term prevention to stay one step ahead.
The best takeaway? Getting expert help early means less hassle, fewer relapses, and healthy nails that never slow you down.
Conclusion
When it comes to toe fungus, paying attention early is your not-so-secret weapon for healthier feet and fewer disruptions to your busy life. The real power lies in taking control before a nagging nail issue turns into something costly or chronic.
Getting proactive means you’re skipping endless cycles of home remedies, safeguarding your mobility, and avoiding stress that no one needs—especially when work and life are nonstop.
Essential Takeaways to Put Into Action:
- Monitor any persistent nail changes—think unusual color, thickening, or nail discomfort.
- Book a specialist appointment promptly if symptoms linger beyond 2–4 weeks or worsen.
- If you’re high-risk (like living with diabetes or a weakened immune system), treat toe fungus as urgent, not optional.
- Track your symptoms and daily impact to streamline conversations with your doctor.
- Don’t just treat—commit to smart prevention habits to stop infections before they start.
What Should You Do Now?
- Check your toenails today—a two-minute self-exam could save you months of hassle.
- If you spot anything unusual, set a calendar reminder to contact your podiatrist—no more “I’ll get to it next week” excuses.
- Review our printable symptom checklist so your next doctor’s visit is quick and productive.
- Share this actionable guide with a friend or colleague who needs to hear it—their future self will thank you.
- Explore our prevention and advanced treatment resources to lock in long-term foot health.
Every step you take—no matter how small—brings you closer to healthier nails and fewer interruptions in your day. Don’t let a minor nail issue steal your focus or slow your stride. The best outcome always belongs to those who act fast and stay vigilant.
Stay engaged, check in, and remember: Healthy feet are the foundation behind every great run, pitch, or presentation. Step up, take action, and keep moving forward.