Key Takeaways
Pinpointing the difference between toe fungus and other foot conditions can save you weeks of frustration—and even prevent unnecessary treatments or complications. Here are the most actionable, real-world insights to help tech-driven professionals and creators catch problems early, address them effectively, and get back to work (or your next workout) with confidence.
- Spot classic signs of toe fungus by looking for yellow or brown nail discoloration, thickening, and crumbly edges—these changes develop gradually over months, not overnight.
- Don’t confuse athlete’s foot with toe fungus—if your issue targets skin and causes itching or burning, it’s likely athlete’s foot; nail discoloration and thickening? Fungus is your culprit.
- Gym showers, sweaty shoes, and shared spaces are notorious for spreading both toe fungus and athlete’s foot—rotating footwear and keeping feet dry are your first defense.
- Quickly differentiate viral (plantar warts), mechanical (ingrown nails), and fungal problems by focusing on location (nail vs. skin), pain type, and unique visual cues—misidentification leads to wasted time and ineffective fixes.
- Tech-powered self-assessment beats guesswork—snap smartphone photos of foot changes, log symptoms and dates, and track progress before your next medical consult.
- Don’t overlook structural foot issues—if you’re battling pain, swelling, or trouble walking (with normal nails), it’s likely a mechanical or nerve problem, not fungus—seek targeted solutions.
- Prioritize medical help if you see sudden color change, pus, swelling, or spreading redness—these are red flags for infection or more serious conditions needing prompt care.
- Use at-a-glance comparison charts to quickly match symptoms to the right condition and treatment, avoiding unnecessary OTC spending and downtime.
A few minutes of smart, informed foot-checking can help you skip weeks of discomfort and lost productivity—explore the full guide for visuals, pro tips, and recovery shortcuts that work for your lifestyle.
Introduction
Ever found yourself squinting at your toes during a morning shower and wondering, “Is this just a bruise, or something serious?” You’re not alone—nearly 1 in 10 adults will face toe fungus at some point, but distinguishing it from a crowded field of foot issues can feel like troubleshooting a vague software error.
Between remote work (hello, barefoot video calls) and gym sessions squeezed between deadlines, today’s tech pros and creators actually run a higher risk for stubborn, confusing foot problems—and the wrong guess can mean weeks of frustration and wasted effort.
What’s at stake goes beyond looks or mild discomfort:
- Wasted money on the wrong treatments (and missed meetings for extra appointments)
- Risk of spreading the problem to other nails or even colleagues—think shared mats and “hot desking”
- Lost productivity when small pains snowball into bigger, longer outages
But here’s the twist: Toe fungus isn’t the only condition trying to grab your attention. Athlete’s foot, plantar warts, ingrown nails, and even simple calluses or blisters can all hide behind similar signs—blurring the line between easy fix and chronic hassle.
So how do you know what you’re up against… and catch it before it turns into a project that eats your time and energy?
This guide breaks down:
- Key differences between toe fungus and common lookalikes (from athlete’s foot to bunions and beyond)
- Real-world triggers unique to digital, on-the-move lifestyles
- The most practical, tech-savvy ways to document, track, and tackle symptoms—before they hit your next sprint or campaign
Think of it as your go-to, jargon-free flowchart for restoring comfort, confidence, and peak efficiency—maybe even before your next status update.
Ready to cut through the confusion? Let’s zero in on the subtle signals and expert strategies that mean faster, smarter foot care—starting with what toe fungus really looks like, and why quick ID can make all the difference.
Understanding Toe Fungus and Why Accurate Identification Matters
Recognizing toe fungus from the start can save you weeks—or even months—of frustration and failed fixes.
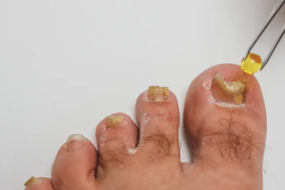
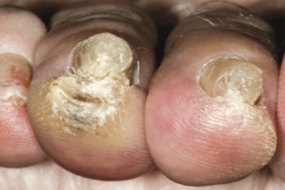
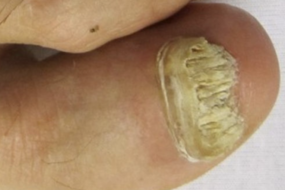
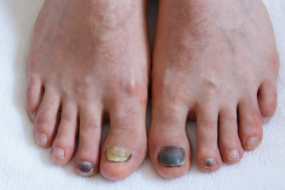
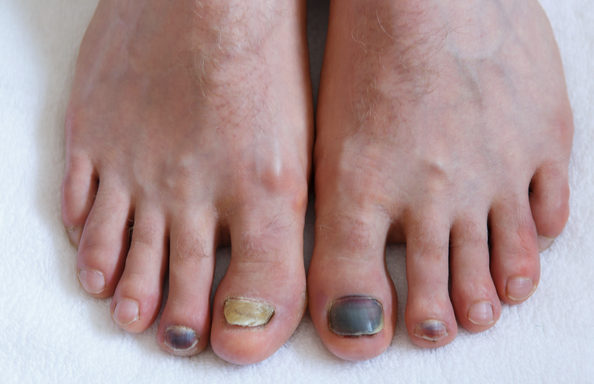
If you've seen your nail turning yellow or brown, getting thicker, or showing brittle, crumbly edges, you're already looking at the most common signs of fungal nail infection.
The Classic Signs: What Toe Fungus Looks Like
You can usually spot onychomycosis (toe fungus) by these key changes:
- Color shifts in the nail—white, yellow, brown, or even green
- Thickening and a rough, uneven nail surface
- Brittleness or chalky, crumbly edges
- Occasionally: the nail lifts away from the bed or partially falls off
These symptoms typically evolve slowly over months, not overnight.
Why Precision Matters—And Fast
Misreading fungus as, say, “just a bruise” or “athlete’s foot” means treatment can drag on—costing you time, co-pays, and endless creams that don’t work.
Misdiagnosis can lead to:
- Delayed recovery and risk of permanent nail damage
- Choosing the wrong over-the-counter products (wasted spend)
- Infecting other nails or people around you
“Identifying toe fungus early prevents the chronic cycle of missed work, shoe struggles, and avoidable medical visits.”
Tech-Driven Lifestyles, Unique Risks
Let’s get practical: if you’re always in sneakers, hot-desking, or clocking miles between coworking spaces, you’re in the club at risk.
- Remote work blurs the line—barefoot at home is common, increasing chill dampness and unnoticed infection time
- Frequent shared showers or gym visits also raise risk—think public locker rooms, yoga studios, camps
Tech-savvy professionals often push through discomfort—sometimes until the infection spreads to multiple nails.
Real-World Confusion: Why It’s Not Always Obvious
Toe fungus loves to play the “great imitator”:
- It gets mixed up with athlete’s foot (a skin issue), viral warts, or even nail trauma from running or tight shoes
- Fungal, viral, bacterial, and mechanical foot problems often look alike at first glance
Picture this: You notice thickened or discolored nails after a busy launch week—was that from running late to meetings in new shoes, or was it lurking communal moisture at your last gym session? The distinction shapes the next steps.
Knowing the classic toe fungus signals—versus other foot woes—lets you act quickly, treat smarter, and get back to peak comfort and productivity. Remember: when in doubt, snap a photo, jot down details, and don’t hesitate to ask a provider for clarity. Early, accurate ID is the best foundation for recovery.
Core Comparison Framework: Toe Fungus Versus Other Fungal Foot Conditions
Toe Fungus (Onychomycosis) vs. Athlete’s Foot (Tinea Pedis)
If you’ve ever swapped out sneakers at the gym and noticed itchy toes or a darkened nail, you’ve met the two most notorious fungal foot foes: toe fungus and athlete’s foot.
Both thrive in warm, damp environments—think sweaty shoes, public locker rooms, or the tile at your coworking space’s shower.
But while they sometimes show up together, their patterns—and management—are strikingly different.
- Toe fungus (onychomycosis):
- Targets nails and nail bed
- Nail looks thickened, yellow/brown, crumbly, may lift off
- Progresses slowly (over months)
- Contagion: Moderate; usually spread from your own skin
- Athlete’s foot (tinea pedis):
- Targets skin between toes, sometimes sole or side of foot
- Appearance: itchy, burning, red, peeling/cracked skin; may blister or smell
- Appears quickly after wet exposure
- Contagion: High; spreads via floors, towels, direct contact
Side-by-side comparison can save you weeks of misdiagnosis and frustration.
“A brittle, discolored nail is toe fungus territory—itchy, shedding skin means athlete’s foot is in the game.”
Shared Risk: Where Both Like to Hide
- Gym showers, pool decks, and shared shoes boost your risk for both
- Sweaty socks and skin cracks are golden tickets for fungus invasion
If you get both at once, treating just one won’t solve the foot puzzle—so combine topical and oral antifungals as a pro tip for lasting results.
Toe Fungus vs. Plantar Warts
Here’s where things get quirky: Toe fungus is a fungal infection, while plantar warts are caused by a virus (HPV).
Picture this:
- Toe fungus: Begins at the nail, causing color change, thickening, and crumbling.
- Plantar warts: Found on the sole, not the nail; look like rough, pebble-like patches with little black dots (capillaries trapped by the virus).
Contagion paths diverge:
- Toe fungus: Likes cracks in the nail/skin, enters through damage
- Plantar warts: Loves broken skin on weight-bearing areas—spreads via showers, pool tiles, yoga mats
What to spot, fast:
- Nail thickening/discoloration? Most likely fungus.
- Painful, pressure-sensitive patch with black dots? Probably a wart.
“Not all foot pains are created equal—pinpoint the difference and you’ll save time, budget, and headaches.”
Immediate takeaway:
Use location and appearance—nail or skin, thickened or bumpy—to guide your next step. When in doubt (or if both show up for the party), connect with a podiatrist before cycling through OTC fixes. Knowing what you’re fighting is the first step to winning.
Toe Fungus Versus Non-Fungal Nail and Skin Disorders
Toe Fungus vs. Ingrown Toenail
If your toe is throbbing, red, and swollen, you might not be dealing with fungus at all. Ingrown toenails are a mechanical problem—think poorly fitting shoes, aggressive nail trimming, or genetic nail shape—not an infection at the start.
Here’s what to watch for:
- Toe fungus changes the look and texture of your nail—yellowing, thickening, and brittleness—but usually lacks sharp pain.
- Ingrown toenails cause localized pain, swelling right beside the nail, and sometimes pus or warmth if a bacterial infection sets in.
If you're seeing redness that spreads or drainage, it’s time to call your doctor; secondary infection can set in fast.
- Fungal infections = contagious to some degree; mechanical issues like ingrown nails = not contagious.
- Treatment differs: fungus needs antifungal medication; ingrown nails may require lifting, minor surgery, or antibiotics if infected.
“Painful swelling and pus? That’s your cue: Ingrown nails mean see a professional—fast.”
Toe Fungus vs. Corns, Calluses, and Blisters
Picture this: you’ve just finished a treadmill session, and now there’s a painful patch or fluid bubble on your toe or heel. Odds are, it’s not a fungus.
Mechanical foot conditions are sparked by pressure, friction, or repetitive movement—not germs.
Here’s how to tell the difference:
- Corns and calluses: hardened, thick skin on pressure points—common in runners, gym-goers, or those in business shoes all day.
- Blisters: fluid-filled sacs caused by friction and new shoes, usually healing with rest.
- Toe fungus: nail-focused, doesn’t resolve if you just swap shoes or apply a blister pad.
At-home care is often enough for corns, calluses, and blisters. But if there’s persistent pain, infection signs, or slow healing, get checked.
“Friction isn’t infectious—if it’s your skin thickening, it’s probably not fungus.”
Toe Fungus vs. Nail Psoriasis and Trauma-Induced Nail Changes
If your nail is thick, crumbly, or separating, don’t jump to fungus right away—psoriasis or trauma can look nearly identical.
Key clues:
- Psoriasis often affects multiple nails, sometimes with pitting (tiny dents) and has a family or personal history—you may notice patches elsewhere on your body.
- Nail trauma (picture dropping a laptop on your foot or repeated stubbed toes) can suddenly discolor or thicken a nail.
- Toe fungus: Usually starts in one nail and spreads slowly—contagious and persistent.
Treatment pathways:
- Toe fungus = antifungal meds, expect months until improvement.
- Psoriasis = anti-inflammatory treatments, not contagious.
- Trauma = mostly waiting it out unless there’s pain or persistent change.
“Thick or discolored nails? One nail and gradual spread suggests fungus, but a history of bumps or family psoriasis should shift your suspicion.”
Knowing which toe or skin changes point to infection vs. injury or genetics can save you months of self-misdiagnosis. If it’s sudden, painful, or there’s a history of trauma or psoriasis, flag it and consider a professional check—right diagnosis, right fix, less time off your feet.
Toe Fungus Compared to Structural and Nerve-Related Foot Problems
Understanding the Difference: Infection vs. Structure
Toe fungus is all about the nail—yellow, thick, crumbly, and sometimes separating from the toe.
By contrast, bunions, plantar fasciitis, neuromas, and arthritis are mechanical or nerve-related issues.
- They attack bones, joints, or nerves, not the nail itself.
- Expect pain, swelling, odd toe angles, and movement trouble, but nails usually look normal.
“Picture this:” A bunion creates a red, bulging bump at your big toe base that aches in tight shoes, while fungal nails look rough and stained but don’t shift the toe’s position.
Symptom Snapshot: What Sets Each Apart?
If you’re troubleshooting foot pain, these core symptoms can help you spot the culprit:
- Toe Fungus:
- Nail thickening
- Yellow/brown discoloration
- Brittleness/crumbly nail edges
- Often, little or no pain
- Structural or Nerve Problems:
- Bunion: hard bump and toe drifting inward
- Plantar fasciitis: stabbing heel pain, especially with first morning steps
- Neuroma: burning, tingling, or “pebble-in-the-shoe” feeling at the ball of the foot
- Arthritis: joint stiffness, swelling, limited big toe motion
Key quotable: “Nail changes point to fungus; pain and movement issues usually mean it’s a structural problem.”
Shoes, Activities & Overlap: Real-World Triggers
Footwear is a classic trigger.
- Tight, narrow shoes crank up bunion and neuroma risk.
- Long hours on your feet—or at a standing desk—increase structural pain and inflammation.
- Shoes that trap sweat can spark fungal infections.
Sometimes, these issues coexist:
- A tech pro with plantar fasciitis could also develop fungus from sweaty sneakers.
- Chronic arthritis may change toe alignment, making fungal nail entry easier.
“Don’t be surprised if your foot has more than one story to tell—pain and odd nails can team up.”
When to Suspect More Than Fungus
If you notice:
- Persistent pain, swelling, or joint stiffness (not just nail changes)
- Trouble walking, burning, or numb toes
…it’s time for a deeper look. Fungal nail treatments won’t fix mechanical or nerve issues—and vice versa.
For tech-driven self-care, track symptoms by snapping smartphone photos and logging pain or swelling patterns. This can speed up professional diagnosis if your at-home fixes stall.
Knowing the difference between toe fungus and structural foot issues is a shortcut to feeling better, faster—and saves you from chasing the wrong solution. If nails change shape or color but you feel real pain when walking or standing, double-check for more than just fungus.
Risk Factors, Overlaps, and When to Get Help
Key Shared and Unique Risk Factors Across Conditions
If you ever wondered why certain foot conditions seem impossible to avoid, you're not alone—shared environments and daily habits are largely to blame.
Some key risk factors for toe fungus, athlete’s foot, plantar warts, and other issues include:
- Warm, moist work environments (think: hours in the same shoes, office carpet, or hot commutes)
- Shared communal spaces like gyms, locker rooms, or hotel bathrooms
- Footwear habits—tight shoes and synthetic socks create petri-dish conditions
- Chronic health issues such as diabetes or vascular disease, which increase susceptibility and slow healing
- Weakened immune systems—long hours, burnout, and packed schedules can make tech pros more vulnerable
- Frequent travel or day-to-day movement from desk to desk, especially in shared environments
“Busy professionals who clock 8+ hours daily in shoes can have double the risk for fungal foot issues compared to those who rotate footwear and let feet breathe.”
Situations Where Symptoms Overlap or Coexist
Now, imagine trying to diagnose: is that itchy, red skin athlete’s foot or the start of something else?
Overlapping symptoms are common and may confuse even seasoned self-assessors. Some common mixed scenarios include:
- Athlete’s foot with toe fungus: itching between toes plus yellow, thickened nails
- Ingrown nail plus infection: local pain and swelling, sometimes with pus or red streaks
- Corns, calluses, or blisters on a background of fungal infection—each can mask the other
Tech-minded readers: treat your foot symptoms like diagnosing a device bug—you want to track:
- Color changes
- Spot location(s)
- Pain level and type (sharp, burning, pressure)
- How quickly symptoms appeared
- Recent exposure to shared surfaces or travel
Practical Advice: Self-Assessment Tools and Red Flags for Professional Care
Harness your device and workflow skills to monitor your feet like a pro.
- Snap smartphone photos when changes start, then log pain level, duration, and appearance
- Use your favorite task app or note system to track daily symptoms
- “If you see sudden color changes, severe pain, pus, or rapidly spreading redness, it’s time to get medical help—no delay”
- Share timeline, pics, and symptom data with your doctor for a “diagnosis-ready” consult
Early, smart differentiation can:
- Save money on ineffective treatments
- Reduce time away from work or important meetings
- Prevent complications before they disrupt your life (and let’s be real, your next deadline won’t wait)
For tech pros and creators, quick action and good records mean less downtime and better results for your feet—just like for your code or content.
Visual and Feature-Based Comparison Charts
Summary Table: At-a-Glance Differences Between Major Foot Conditions
If you’re juggling remote meetings or managing a busy schedule, a fast, visual breakdown is your best friend for foot health. Here’s a table you can scan in seconds—think of it as your quick-reference cheat sheet.
Pro Tip: Take smartphone photos of your foot issue for easy symptom tracking—this hack saves time at your next telehealth appointment.
How to Use This Chart in the Real World
- Need a lightning-fast check? Locate your symptoms in the Appearance and Key Symptoms columns for instant self-assessment.
- Not sure if it’s contagious? Focus on the Contagion Risk row—if it’s high, take extra care in shared environments.
- Curious about home care steps? The Recommended Steps column gives clear, actionable next actions, whether you need an over-the-counter cream or should swap out those office shoes.
When Details Matter: Linked Guides for Deeper Dives
If a cell above matches what you’re seeing, tap over to our linked guides for:
- Photo walkthroughs of each condition
- Latest treatment timelines and effectiveness rates
- Common mistakes to avoid when self-treating
Remember: “The difference between toe fungus and a callus can be subtle at first—but the right treatment depends on your detective skills.” If your symptoms are unclear, record trends and ask a provider early—catching issues at the right moment can mean the difference between a quick fix and a lasting problem.
When you’re seeing signs that overlap (maybe a thick nail and burning skin?), tracking both—preferably with images and a symptom diary—will streamline your professional consult and speed up recovery. Your data is your diagnostic superpower—especially if your weekdays are packed.
Conclusion
Identifying toe fungus quickly—and distinguishing it from other foot conditions—puts you in control of your comfort, productivity, and peace of mind. With the right knowledge, you can skip the trial-and-error, target your treatment, and dodge unnecessary downtime.
Your next steps aren’t just about healthier feet—they’re about saving time, avoiding recurring hassles, and keeping your momentum strong, whether you’re on the move or clocking in remotely.
Key takeaways to boost your foot health today:
- Document symptoms with smartphone photos—visual records clarify what’s changed and help your provider diagnose faster.
- Match what you see to the right category: nail changes point to fungus, skin issues could be athlete’s foot or warts, and pressure spots often signal mechanical problems.
- Don’t second-guess stubborn symptoms—if pain worsens, you spot pus, or self-care stalls, connect with a provider for prompt care.
- Rotate shoes and let your feet breathe; technology doesn’t slow down, but fungal infections will if you don’t.
Action plan for immediate progress:
- Check your nails and feet in good light tonight; use the comparison chart as a cheat sheet.
- Log any changes, pain, or exposure risks in your notes app.
- Schedule a quick telehealth or in-person consult if anything is unclear—your future self (and your favorite shoes) will thank you.
Every well-diagnosed symptom is a win—more clarity, less guesswork, and real running room for your goals.
Give your feet the same proactive care you bring to your workflow—because small steps make all the difference in the path ahead.