Key Takeaways
Nail psoriasis goes far beyond appearance—it’s your immune system talking, and choosing the right strategy brings both relief and confidence. Here’s your rapid-fire playbook for understanding, treating, and managing nail psoriasis with practical, actionable care.
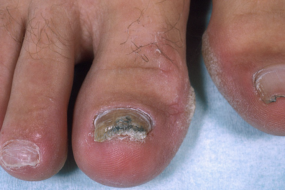
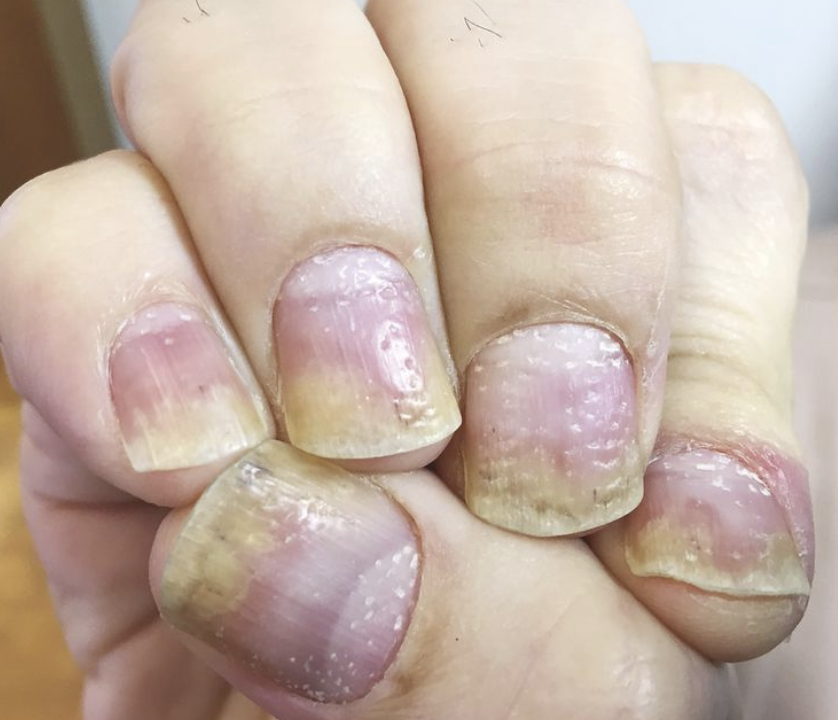
- Spot nail psoriasis early by watching for tiny pits, yellow discoloration, and lifting (onycholysis)—catching these subtle changes early can jumpstart effective treatment.
- Get an accurate diagnosis—if antifungals aren’t working or you see multiple changes, consult a dermatologist to avoid wasted time on the wrong treatments.
- Topical treatments (steroids and vitamin D creams) deliver up to 90% improvement for mild cases, but require consistent, daily use for at least 3–6 months to see real results.
- Intralesional corticosteroid injections target stubborn nail changes, achieving up to 91% smoother nails within a few brief, in-office sessions.
- Systemic and biologic therapies are game-changers for severe or multi-nail involvement, producing over 50–89% improvement—especially if you have skin or joint symptoms too.
- Smart daily routines—short nails, heavy moisturizers, and gloves during chores—are your best defense against triggers and slow progress, helping prevent both flares and infections.
- Latest innovations like JAK inhibitors, microneedle patches, and advanced lacquers are unlocking faster, more targeted relief—ask your doctor about new trials or delivery methods.
- Personalize your plan in partnership with your care team: Track symptoms, set goals, and review progress every 3-6 months to keep your treatment on track for visible, meaningful improvements.
Nail psoriasis relief is all about consistent care and choosing the right approach—dive into the full article to see how science, strategy, and small daily wins add up to stronger, healthier nails.
Introduction
Ever glanced at your hands in a meeting, only to spot yet another new dent or odd yellow streak on your nails—then wondered if it’s just wear-and-tear or something more? More than 50% of people with psoriasis will develop nail changes at some point, yet many tech-savvy professionals still chalk it up to stress or bad luck.
If you’re navigating client calls between coding sprints—or just typing at warp speed—there’s little room for nagging discomfort on your fingertips. Nail psoriasis doesn’t just affect appearance; it can disrupt routines, spark self-consciousness, and—if missed—impact your overall health. The silver lining? There are strategies and real solutions within reach that respect your time and maximize your results.
You’re here because you want more than quick fixes. You want:
- Real clarity: Know exactly how to spot nail psoriasis and catch it before it derails your week
- Practical, proven treatments: From high-impact topicals to tech-forward therapies
- Actionable daily routines: Small upgrades that keep your nails—and confidence—on track
- A roadmap to new research: What’s on the innovation horizon, and how can you benefit next?
Think of this as your insider’s playbook—a blend of expert strategies, efficiency tips, and confidence boosts tailored for busy, tech-empowered professionals.
You’ll get digestible guidance for everything from symptoms to smart self-care. Plus, you’ll understand why those nail changes are sending critical signals about your immune system—and how addressing them now sets you up for all-around wellness.
So, what’s really happening beneath the nail surface? Let’s peel back the layers and see what your nails are telling you, starting with a clear-eyed look at what nail psoriasis looks like from the inside out.
Understanding Nail Psoriasis: What You Need to Know
Nail psoriasis isn’t just a cosmetic issue—it’s your body’s immune system making itself visible in real time.
Picture this: your fingernail is like a tiny billboard for inflammation, quietly telling a bigger story about your health.
Nail Psoriasis Basics: What’s Actually Happening?
Nail psoriasis is an inflammatory condition where your immune system confuses healthy nail tissue for an invader. This results in:
- Pitting: Tiny dents peppering the nail surface
- Ridging: Grooves running lengthwise or across the nail
- Discoloration: Ranging from yellow-red (“oil spots”) to chalky white patches
- Onycholysis: When the nail pulls away from the bed—look for a gap or a white tip that’s too big
- Thickening: The nail builds up more layers and feels tough
- Subungual debris: Yellowish material collecting under the nail
These symptoms can hit one nail or all ten—sometimes toes get roped in, too.
“If you spot random pits or notice your nail lifting, it could be more than a simple infection.”
What Makes Nail Psoriasis Different From Other Nail Problems?
It’s easy to confuse nail psoriasis with fungal infections or eczema.
- Fungal infections usually involve more crumbly, yellow nails and sometimes itch; lab tests will show fungus.
- Eczema may make the skin around the nails red or scaly, but rarely causes deep pits or separation.
If over-the-counter antifungals don’t work, or you see several nail changes at once, a dermatologist can help sort it out.
Why Nail Psoriasis Gets Missed
Surprisingly, nail psoriasis is misdiagnosed up to 50% of the time because its symptoms mimic other common nail conditions.
Doctors may miss it if you don’t have obvious skin plaques—yet nail psoriasis can be your only sign. Even tech-savvy readers may assume it’s just “bad nails”—then slog through months of useless creams.
The Bigger Picture: Nail Health and Your Immune System
Think of nail changes as your body waving a small red flag.
- Nail psoriasis can be the first clue to psoriatic arthritis, which affects up to 30% of people with psoriasis.
- Regular nail changes can signal that your immune system’s working overtime—timely care can prevent bigger issues.
If you notice new dents, thickening, or color shifts that don’t go away, it’s time for a closer look.
Spotting changes early, tracking what you see, and knowing when to seek help is the first big step. Your nails aren’t just decoration—they’re powerful messengers about your health.
Recognizing Nail Psoriasis: Signs, Progression, and Diagnosis
Signs to Watch For
Nail psoriasis is like reading your body’s signals in real time—if you know where to look.
Watch for these quick, tell-tale signs on your fingernails or toenails:
- Pitting: Tiny dents or dimples—think of pin-sized dots splattered on the nail surface.
- Discoloration: Yellowish or brownish patches beneath the nail, sometimes described as an “oil-drop” effect.
- Subungual hyperkeratosis: Thick, crumbly, or yellow material building up under the nail—this one’s a classic.
- Onycholysis: The nail lifts away from the nail bed, creating a gap that can appear white or yellow.
- Ridges and thickening: Vertical or irregular grooves, often with noticeable overall thickening.
- Crumbly edges or splitting: Far beyond everyday wear-and-tear.
You might see just one or two nails affected—or all twenty over time.
It's common for symptoms to start subtly and progress slowly, so early changes are easy to overlook.
Simple At-Home Checks
Try these tips to spot early patterns:
- Examine each nail under bright light—compare any differences in color, thickness, or texture.
- Tap the surface with a pen cap: if it feels bumpy or uneven, pitting is likely.
- Look for white/yellow separation at the tips; gentle pressure shouldn’t hurt, but nails may feel soft or loose.
“Picture this: You compare both hands, and your dominant hand’s nails have more pits—psoriasis frequently picks favorites.”
Getting the Right Diagnosis
Getting a correct diagnosis starts with a detailed medical history and a close physical exam.
Here’s what a thorough work-up might include:
- Visual inspection and gentle tapping for pitting or ridges.
- Ruling out fungal mimicry by sending nail clippings for culture or sometimes a biopsy.
- Asking about any skin rashes or joint pain, since these influence treatment options.
Your dermatology provider will check for psoriasis elsewhere (elbows, scalp, knees) and might ask about family history.
Don’t self-diagnose—fungal infections and eczema can look eerily similar. Treatments differ completely.
Why Accurate Diagnosis Really Matters
Misdiagnosed nail psoriasis leads to years of wasted time and frustration—over 50% of people with psoriasis experience nail changes, but up to half are initially missed or mistaken for fungus.
Facing visible nail changes can trigger real emotional stress, especially for tech pros or anyone whose work puts hands on display.
“Every nail tells a part of your health story—don’t let mixed signals slow down the right treatment.”
Accurately identifying nail psoriasis is the first crucial step toward relief, better nail health, and stronger confidence day-to-day.
Treatment Options for Nail Psoriasis: What Works and When
Topical Treatments: The Frontline for Mild Cases
When it comes to mild nail psoriasis, think of topical treatments as your automatic go-to. They’re easy to use, widely available, and deliver real results—especially if you catch symptoms early.
Here’s the powerhouse trio you’ll want to remember:
- Corticosteroids (like clobetasol propionate): Tackle pitting, ridging, and nail separation. Studies show up to 90% improvement if you stick with it.
- Vitamin D analogs (calcipotriol): Perfect for nail discoloration and subungual debris. Massage into cuticles or beneath the nail edge twice daily.
- Retinoids (tazarotene): Smooth out pits and yellowing when used under light wraps or “occlusion.”
Combination therapies (for instance, a topical steroid plus calcipotriol) can boost results—up to 75% NAPSI score reduction after 6 months. Patience pays off: it often takes half a year to notice marked change, thanks to slow nail growth.
Supporting topicals you might try:
- Calcineurin inhibitors (tacrolimus) for thin, sensitive skin
- Keratolytics (urea or salicylic acid) to smooth thickened nails
“Consistent application for months unlocks visible improvement—think marathon, not sprint.”
Intralesional Corticosteroid Injections: For Stubborn Nails
When topicals hit their limit—especially with deep pitting or thick ridges—your doctor may suggest injections directly into the nail fold.
- Expect a small dose of triamcinolone (5-10 mg/ml) every 4-8 weeks
- These target the nail matrix itself, shrinking pits up to 91% and smoothing ridges in about 83% of cases
The procedure is quick but can be briefly painful. Side effects? Mostly minor—bruising or achy fingers—while rare risks include temporary nail thinning or loss.
Picture this: a brief sting at the doctor’s office, weeks of smoother nails on the other side.
Systemic and Biologic Treatments: For Severe, Multi-Nail, or Skin/Joint Disease
If multiple nails, skin plaques, or joint pain are involved, it’s time to talk “whole body” solutions.
Options include:
- Biologics: Targeted, high-response medications (like secukinumab, adalimumab, ustekinumab), delivering over 50-89% nail improvement in trials
- Traditional systemic drugs: Methotrexate, cyclosporine, and acitretin—practical, but with more side effects and monitoring (Nail improvement: 37-89%)
- Phototherapy (PUVA) or, rarely, surgical nail removal, for the most stubborn cases
“If your nails are only part of the story, systemic treatment may offer bigger-picture relief.”
Cost, Access, and Decision Factors
Treatment choice often boils down to:
- Severity: Mild = topicals; severe = systemic or biologics
- Number of nails affected
- Co-existing skin/joint symptoms
- Lifestyle and cost: Biologics offer impressive results but can mean higher out-of-pocket costs—though insurance often covers severe cases
Plan on 6+ months for major visible change; instant fixes simply don’t exist for nails.
The big picture: You have real options, but it’s about matching the right tool to your unique situation—and playing the long game with steady, consistent care. Remember, “slow and steady” truly wins in nail psoriasis relief.
Practical Home Care and Daily Strategies for Nail Health
Keeping your nails healthy with psoriasis isn’t rocket science, but it does call for a smart daily routine. A few small habits make a world of difference—and consistency beats intensity every time.
Start With the Basics: Your Low-Maintenance Nail Routine
- Keep nails short and smooth—it prevents snags and trauma that trigger flares.
- Gently file the edges with a fine emery board to reduce splits.
- Moisturize hands and nails after every wash using a thick, fragrance-free cream; lock in hydration by wearing cotton gloves overnight if you’re feeling ambitious.
- Wear waterproof gloves when cooking, cleaning, or gardening. Anything that soaks or irritates nails can set you back weeks.
Make this your non-negotiable checklist: short, smooth, moisturized, and protected.
Watch Out for Triggers: Trauma, Biting, and Chemicals
- Avoid harsh chemicals— acetone, cleaning agents, and even frequent alcohol-based hand sanitizers can dry and irritate.
- Resist the urge to bite, pick, or peel at nails or cuticles. Replace the habit with a stress ball or keep a bottle of bitter-tasting nail polish on hand for those fidgety moments.
- Skip artificial nails and acrylics—these traps moisture and worsen separation.
A single slip—biting or slamming your hand on a desk—can undo months of progress. “Think of each nail as a slow-moving project: patience pays off.”
Appearance Boosts While You Heal
- Buff gently to smooth ridges but never dig into the nail plate.
- Prefer breathable, “nail-friendly” polishes and acetone-free removers if you want to polish up. Avoid gel or dip powders that require aggressive removal.
- Hide imperfections with a sheer tint, but always let nails breathe between applications.
Pro tip: Even after visible improvement starts, nail growth is slow—6 months or more for a full renewal, according to clinical data.
DIY Hacks & Infection Prevention
- Use a stress ball or fidget toy to redirect nervous energy away from your hands.
- Moisturize cuticles—not just tips—to support healthy growth.
- Check for redness, swelling, or thickened nails—a quick call to your dermatologist if you spot infection can save you serious trouble.
Picture this: running your thumb over a nail that’s finally smooth and pain-free. That’s your small-win moment—celebrate it.
Ongoing nail health with psoriasis is about the little wins stacking up over months, not weeks. Stay consistent and don’t sweat the setbacks—progress in nail psoriasis is slow, but every bit counts.
Latest Innovations and Research in Nail Psoriasis Treatment
Picture this: you’re staring down stubborn nail psoriasis, and the usual creams just aren’t cutting it. Good news—new therapies are racing ahead, reshaping what “treatable” really means.
Breakthrough Medications: Beyond the Basics
The research spotlight is on small molecule drugs and targeted immune therapies. These include:
- JAK inhibitors (like tofacitinib and upadacitinib): Early studies show nail improvement rates of 60–70%, offering hope for tough cases.
- Next-generation biologics: Think risankizumab or ixekizumab—delivering >50–89% NAPSI improvement (that’s the gold-standard nail severity score), especially when skin or joint psoriasis tags along.
“Patients in recent trials saw visible nail improvements in just 12–24 weeks—light speed compared to traditional options.”
Delivery Innovations: Smarter, Faster Results
Cutting-edge drug delivery tech is making waves, helping medications actually reach the nail bed.
- Advanced nail lacquers: Specialized formulas lock treatments onto and under nails for longer wear.
- Microneedle patches: Tiny, almost painless arrays bypass the hard nail plate and deliver medication deeper than ever before—think of it as “express shipping” for your prescription.
- Ultrasound-assisted delivery: Still experimental, but early results suggest up to 30% better penetration versus ointment alone.
“Innovative lacquers and microneedles are unlocking faster, more targeted relief—nail care is finally catching up to skincare.”
Research Pipeline: What’s Next?
Clinical trial momentum is strong. Here’s what’s bubbling up:
- Ongoing trials for oral TYK2 inhibitors and new topical agents promise more options for patients whose nails resist everything else.
- Combination regimens (like biologic + topical) are proving especially effective in head-to-head studies—some report 75%+ improvement within six months.
- Pay attention to new trial announcements—eligible patients could access tomorrow’s treatments today, often at no cost.
“Ask your dermatologist: ‘Are there any trials for nail-specific psoriasis? I’m ready to try what’s next.’”
Curious about what’s on the research horizon? The trend is clear: better results, fewer side effects, and smarter delivery are on the way. If you’ve struggled with traditional care, now’s the time to talk options—your best nails may still be ahead of you.
Working with Your Care Team: Personalizing Your Treatment Plan
Navigating nail psoriasis isn’t a solo project—you’ll get better, faster results with the right team on your side.
The first step? Find a dermatologist who truly understands the nuances of nail psoriasis—not every skin specialist does.
It’s worth asking up front about their experience treating nail-specific symptoms and biologic therapies.
Prep Smart for Appointments
Come prepared, so you and your dermatologist can make every minute count. Use these power moves:
- Track your symptoms: Note flare-ups, triggers, and nail changes in a phone app or journal.
- Bring photos of your nails over time, especially if they change more quickly than visits happen.
- List every treatment you’ve tried (and how long), from prescription creams to home remedies.
This data-driven approach ensures you’re not relying on memory and helps pinpoint what’s moving the needle.
Collaborate—Don’t Just Receive Directions
Think of your care plan as a partnership, not just a prescription pad. Come ready to:
- Ask about all options: Topicals, injections, biologics—how do they fit your lifestyle or work demands?
- Advocate for your comfort: If you need gentler methods or worry about side effects, speak up.
- Set expectations together: Discuss realistic nail growth timelines (6+ months for visible results), common side effects, and what progress actually looks like.
The most empowered patients get the most responsive care.
Set Goals and Revisit Regularly
Nail care isn’t just about looks—it’s about living well. Make sure your plan targets:
- Quality-of-life upgrades (less pain, better function, easier hand use)
- Appearance-focused milestones (smoother nails, less discoloration)
- Check in every 3-6 months to review progress and pivot as needed
Celebrating every small win keeps morale up when improvement feels slow.
You’re Not Alone: Progress Happens in Steps
“Picture this: six months from now, your nails are smoother, your morning routine is simpler, and flare-ups are rare. That’s the power of teamwork with the right provider.”
Your top takeaway: being proactive, communicative, and goal-driven with your care team accelerates real progress—even if you’re still waiting on perfect nails.
Nail Psoriasis and Whole-Body Wellness
Nail psoriasis is more than just a cosmetic challenge—it’s a direct reflection of how your immune system is behaving throughout your body.
Those nail changes? They’re signaling underlying inflammation that can increase your risk for other conditions, like psoriatic arthritis, heart disease, and even depression.
Think of your nails as a health dashboard, giving you real-time feedback.
The Bigger Picture: Comorbidities That Matter
Research shows that up to 30% of people with nail psoriasis will develop psoriatic arthritis at some point. Mental health concerns—like anxiety and low self-esteem—are also common, especially when nail changes affect daily activities or social confidence.
But here’s the good news: Focusing on your nails can inspire positive steps for your whole body.
Picture this: When you prioritize nail health, you’re actually supporting your joints, heart, and mind—it’s all connected.
Lifestyle Modifications for Real Impact
Small changes in your daily routine translate into measurable benefits:
- Manage stress with mindfulness, breathing exercises, or even just a daily walk—chronic stress is a known trigger for psoriatic flares.
- Prioritize good sleep hygiene; lack of rest can worsen inflammation.
- Moisturize often, wear gloves for chores, and avoid nail trauma—studies show these habits reduce both flares and infection risk.
- Eat a balanced diet low in processed foods, which may ease inflammation for some.
You can think of this as optimizing an “all-systems workflow”—your inputs (daily habits) affect every output (including nail health).
Holistic Nail Care: More Than A Minor Detail
Treat your hands like you do your teeth: routine, mindful care pays dividends.
Try these everyday strategies:
- Keep nails trimmed short and files gentle.
- Use rich creams or ointments, especially after washing.
- Avoid biting, picking, and harsh chemicals (like acetone or strong cleansers).
- Celebrate small wins—nails may grow slowly (think 6-12 months), but every new millimeter is a step forward.
See Nail Care As Essential Self-Care
If you remember only one thing, let it be this: caring for your nails is self-care for your entire body.
“Nail health is whole-person health—if you help your nails, you’re helping yourself.”
By integrating mindful nail care, stress management, and healthy routines, you’re not just treating a symptom—you’re building a foundation for resilience and confidence that goes far beyond your fingertips.
At-a-Glance Reference: Treatment Efficacy, Side Effects, and Timelines
Picture this: You’re chatting with your dermatologist and want a clear, concise cheat sheet for nail psoriasis treatment options, how quickly they work, and what to expect along the way.
Let’s give you the ultimate quick-reference—perfect for decision support and smart conversation with your care team.
Key Therapy Snapshots: Who, What, and When
Here’s your rapid-fire rundown of the major options for nail psoriasis:
- Topical Treatments (creams, lacquers)
- Best if: You have mild symptoms or just a few affected nails.
- Response rate: 50–90% improvement in studies.
- Timeline: Results start after 3–6 months—think “slow and steady.”
- Side effects: Skin thinning, irritation, rare pigment changes.
- Intralesional Steroid Injections
- Best if: Nail pitting, thickening, or ridging is the main concern.
- Response rate: 46–94% for matrix (growth zone) change.
- Timeline: Visible improvement expected after 2–3 sessions, spaced 4–8 weeks apart.
- Side effects: Temporary pain, bruising (up to 20%), rare nail changes.
- Systemic Medications (methotrexate, cyclosporine, acitretin, apremilast)
- Best if: Multiple nails affected or co-existing skin/joint disease.
- Response rate: 37–89% NAPSI improvement.
- Timeline: Noticeable changes in 3–6 months.
- Side effects: Immune suppression, liver impacts, require regular blood tests.
- Biologics (anti-TNF, anti-IL-17, anti-IL-12/23)
- Best if: Severe or stubborn nail involvement, especially with skin/joint issues.
- Response rate: Over 50–89% NAPSI reduction.
- Timeline: Major nail changes within 6 months (sometimes faster).
- Side effects: Injection or infusion site reactions, rare infection risk, high cost.
Compare At-a-Glance: Table Format
Beyond the Data: Quick Takeaways
- “Expect progress, not perfection—nails grow slowly, but improvement adds up.”
- “Combination topicals (steroids + vitamin D) get 75% better results for more severe nails.”
- “If you’re seeing little change after 6 months: time to discuss systemic or biologic options.”
Bottom line: Use this visual guide to track options, set realistic timelines, and ask focused questions. Having a snapshot in hand helps you steer the conversation and celebrate small milestones on your way to healthier nails.
Conclusion
Navigating nail psoriasis doesn't have to mean settling for frustration or hiding your hands. With the right care, a clear strategy, and proactive habits, real relief and healthy nails are within reach—even if progress takes time.
What sets successful nail psoriasis management apart? It’s all about smart, consistent daily routines and leveraging advances in treatment to match your personal needs. You have genuine control over your nail health—every small action today builds confidence for tomorrow.
Here’s what moves the needle most:
- Monitor your nails weekly—snap photos and track symptoms for earlier intervention.
- Prioritize gentle, daily moisturization after every hand wash; it’s your best front-line defense.
- Protect nails from trauma and chemicals by keeping them short and wearing gloves for messy tasks.
- Engage your dermatologist proactively—bring data, photos, and specific questions to tailor your plan.
- Ask about next-gen treatments or clinical trials if standard options stall your progress.
Ready to take the next step?
- Audit your nail care routine today—add at least one protective habit.
- Schedule a check-in with your provider, especially if you haven’t seen change in six months.
- Explore local clinical trials or discuss advanced therapies if you want to stay on the cutting edge.
Your nails can become a source of confidence—not just a health signal. Progress may be measured in millimeters, but every mindful step gets you closer to resilience, function, and pride in caring for yourself.
“Your next great breakthrough could start with a single day’s routine—stronger nails, renewed confidence, and proof you can tackle even stubborn challenges head-on.”