Key Takeaways
Ready to cut through the coding confusion for toe fungus? Here’s your fast-track summary—smart, actionable, and perfect for anyone juggling medical billing, clinic workflows, or even AI automation. Scan these essential points to instantly sharpen your ICD-10 knowledge and minimize claim drama.
- Use B35.1 for confirmed toenail fungus—this universal ICD-10 code covers onychomycosis of both fingernails and toenails, ensuring precise documentation and faster insurance approvals.
- Get specific with companion codes like B35.3 (athlete’s foot), L60.2 (onychogryphosis), and L03.031 (cellulitis)—precision here slashes denials and streamlines the billing process.
- Lab confirmation boosts code accuracy—KOH prep or fungal cultures not only confirm diagnosis but also back up coding for costly treatments or oral meds.
- Rich documentation drives reimbursement—always state location, laterality, number of nails affected, and any related complications or pain for bulletproof claims.
- Avoid unspecified codes at all costs—payers scrutinize vague entries like B49 or B35.9, so anchor every claim in the most detailed code possible for hassle-free approval.
- Tie in chronic risks and comorbidities—add codes for diabetes (E11.9) or PAD (I70.203) to reflect higher risk, justify interventions, and unlock expanded coverage.
- Tech-savvy workflows mean fewer delays—using EMR/AI tools to cross-check codes and documentation can reduce claim denials by up to 35% and keep your admin time lean.
- Strategic ICD-10 coding fuels better care—each accurate entry powers smarter treatments, more effective follow-ups, and empowered patient conversations.
Master these strategies and watch claim approvals, billing efficiency, and patient care all get a serious upgrade—dive into the full article for expert real-world tips you can use immediately.
Introduction
Ever had a claim for a simple toenail fungus treatment bounce back just because of a code mix-up? You’re not alone—coding errors cause up to 35% of fungal nail claims to be delayed or denied, and the tiniest slip can mean weeks of paperwork for you, your team, and your patients.
Suddenly, that “minor” diagnosis turns into a major hassle—and no one has time for that.
If you’re navigating the maze of ICD-10 codes, getting it right isn’t just about correct documentation. It’s the secret to:
- Faster insurance approvals and fewer denials
- Accurate billing that helps you get paid on time
- Better patient experiences—less friction, more trust
And in a world where AI-powered EMRs and payers are scanning every detail, extra precision pays off. The right code doesn't just clear payment hurdles; it signals your professionalism while future-proofing your workflows.
But let’s be honest: “ICD-10 for toe fungus” may not sound thrilling—until you see how a missing detail can tank your reimbursement or leave patients in limbo for needed antifungal therapy.
So why does this matter for you, especially if you’re building smarter processes or training up a tech-driven team?
Because mastering the nuances—knowing that B35.1 covers both fingernails and toenails, spotting when a companion code powers up your claim, or understanding how documentation closes gaps—is the simplest way to keep care moving and headaches to a minimum.
Curious how to turn precise coding into a competitive advantage and keep your billing team (and patients) happy?
You’re in the right place—next, we’ll demystify the essentials of ICD-10 coding for toe fungus, from spotting the right codes to real-world use cases that streamline every encounter.
Understanding ICD-10 Coding for Toe Fungus
When it comes to medical records, ICD-10 codes are the universal language providers and insurers use to describe diagnoses.
Every healthcare encounter relies on these codes to ensure clear documentation, accurate billing, and proper care tracking—whether you’re at a busy clinic or running a solo practice.
Picture this: A digital chart clicks open and a single typo in a code could mean the difference between treatment approved instantly and an insurance denial that sits unresolved for weeks.
What Is ICD-10 and Why Does It Matter?
ICD-10 stands for the International Classification of Diseases, 10th Revision—a global system for classifying health conditions.
This set of alphanumeric codes:
- Standardizes diagnosis reporting across providers, payers, and healthcare systems
- Drives insurance claims, audits, and approval decisions
- Impacts everything from prescription coverage to public health statistics
If you want your antifungal medication covered or your treatment justified, using the right ICD-10 code is step one.
The Go-To Code for Toenail Fungus: B35.1
For toenail fungus, the primary code you’ll use is B35.1—Tinea unguium (onychomycosis).
This site-agnostic code covers:
- Onychomycosis
- Dermatophytosis of nail
- Ringworm of nails
- Dermatophytic onychia
B35.1 applies equally to fingernails and toenails; your documentation, not the code, specifies which are affected.
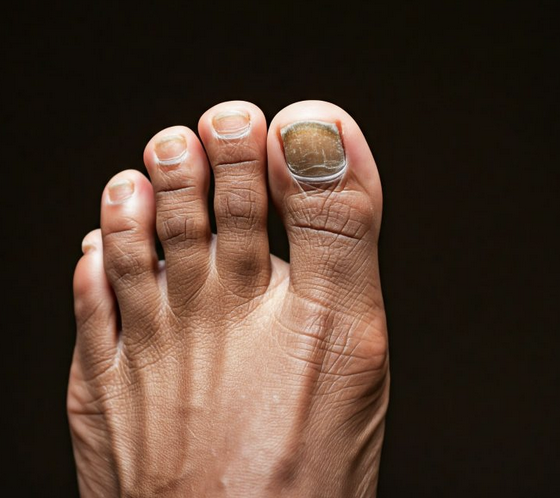
A classic scenario: You chart “thickened, yellow right hallux toenail—fungal debris noted.” The code? Still B35.1.
Differentiating Codes: Getting Specific
If the fungal infection is on the foot skin but not the nail, use:
- B35.3 (Tinea pedis, or athlete’s foot)
For nail problems without confirmed fungus, or for advanced deformities, consider:
- L60.2 (Onychogryphosis)
- L60.3 (Nail dystrophy)
Specificity pays off: Denials often pop up when providers use non-specific codes like B35.9 (fungal infection, unspecified) or B49 (mycosis unspecified) when richer detail is available.
The Bottom Line: Precision Is Power
Think of your ICD-10 code as your key to unlocking coverage, closing care gaps, and proving medical necessity—not just ticking a box.
Accurate coding for toe fungus isn’t just paperwork; it’s the hidden engine that speeds up approvals and keeps your patients moving—literally and financially. In an era where every claim is scrutinized, code with care, document with detail, and expect fewer billing headaches down the road.
Key ICD-10 Codes Related to Toe Fungus
Primary and Companion Codes
When it comes to billing or documentation for toenail fungus, you’ll almost always reach for a single code first: B35.1 – Tinea unguium (onychomycosis).
This code is your go-to for any confirmed fungal nail infection—whether it hits the toes or the fingers.
It’s considered site-agnostic, meaning the same ICD-10 applies regardless of which nail is involved.
Picture this: a patient with thick, yellow toenails and positive KOH prep—you’d list B35.1 as your primary diagnosis.
But real-world toes are rarely so simple. Here’s how companion codes stack up:
- B35.3 – Tinea pedis: Use for athlete’s foot when skin and nail are both affected.
- L60.2 – Onychogryphosis: For those twisted, “ram’s horn” nails, especially long-standing or severe fungus.
- L60.3 – Nail dystrophy: When the diagnosis isn’t confirmed as fungal; think trauma or other nail disorders.
- L60.0 – Ingrowing nail: If ingrowth is the main issue, not fungus.
- L03.031 – Cellulitis of toe: If bacterial infection sets in.
- M79.674 (right toe pain)/M79.675 (left toe pain): For documenting discomfort linked to severe cases.
- Systemic risk? Add E11.9 (diabetes) or I70.203 (peripheral arterial disease) as needed.
Avoid unspecified codes (like B35.9 or B49) when you can pin down the culprit. Payers scrutinize vagueness—specifics mean faster approvals and fewer headaches.
“The more accurate your coding, the smoother your claims process.”
“If it’s not documented, it didn’t happen—at least as far as insurance is concerned.”
Strategic Coding Scenarios
Let’s get practical: imagine a standard podiatry visit for a patient with thickened, yellow toenails and scaling between the toes.
Here’s how the code grouping might look:
- B35.1 (onychomycosis)
- B35.3 (tinea pedis)
Now, picture a primary care encounter with a diabetic patient and foot pain due to fungal nails plus infection risk:
- B35.1 (onychomycosis)
- E11.9 (type 2 diabetes)
- L03.031 (cellulitis, if present)
- M79.674 or M79.675 (toe pain, as needed)
Documentation drives the coding.
For every symptom, complication, or risk factor, record details in the chart to justify each code and avoid claim denials.
Payer policies vary: some plans require proof of fungal confirmation (lab test or photo), while others accept classic visual diagnosis before authorizing pricey oral antifungals.
“Smart ICD-10 pairing tells the full story—and gets you paid for the care you truly deliver.”
The takeaway: precision in coding equals efficiency and less patient frustration.
If you’re building an AI workflow or training your team, double down on specificity—because in the world of medical codes, detail is power.
You’ll unlock faster billing, better outcomes, and fewer insurance callbacks, one accurate toe fungus code at a time.
Clinical Diagnosis: Identifying and Confirming Toenail Fungus
Signs and Symptoms
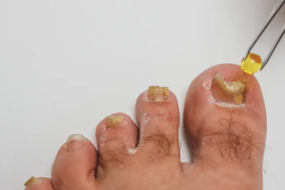
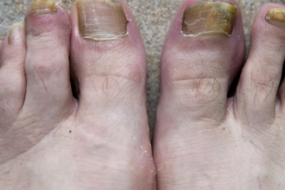
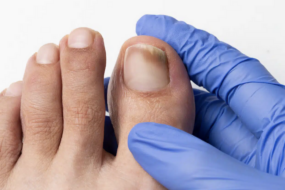
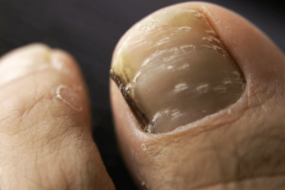
Recognizing toenail fungus early starts with a sharp eye for its telltale signs.
Picture this: you notice a toenail turning yellow or brown, starting to look thick or crumbly, or even lifting away from its bed—a process called onycholysis.
Patients often report:
- Discoloration (yellow, brown, or even white spots)
- Thickened, brittle, or crumbling nails
- Onycholysis – nail separating from the skin underneath
- Subungual debris (chalky material under the nail)
- Sometimes, pain or trouble fitting shoes
But here’s the catch—similar nail changes can show up with:
- Trauma (e.g., stubbing a toe)
- Psoriasis (pitted, thickened, or discolored nails)
- Eczema or unrelated nail dystrophies
You’re not just matching symptoms—you’re a detective sorting clues.
“Discoloration + thickening ≠ always fungus”—every abnormal nail deserves a closer look.
Diagnostic Best Practices
Confirming a diagnosis of onychomycosis is more than a quick glance.
Clinically, seasoned providers may diagnose on sight, but lab confirmation is gold, especially ahead of oral antifungal therapy.
Think about using:
- KOH prep in the office (a fast, affordable test)
- Fungal cultures for more stubborn or unclear cases
- Advanced mycology labs (PCR) for highly accurate identification
Lab-proven fungus impacts coding precision and can sway insurance approval for costly medications.
If the diagnosis is uncertain, you may use:
- L60.3 (Nail dystrophy) if fungal involvement isn't confirmed
- Shift to B35.1 for confirmed fungal nail infection
”A lab slip today means a smoother billing process tomorrow.”
Role of Associated and Complicating Factors
Your chart tells the real story—a simple fungal infection or something bigger?
Always check for:
- Tinea pedis (athlete’s foot): Code B35.3 if both skin and nails are involved
- Cellulitis secondary to the broken nail plate (code L03.031)
- Diabetes or vascular issues: Add codes like E11.9 (diabetes) or I70.203 (PAD) to document risk and support coverage
When non-fungal causes are suspected—psoriasis, trauma, or eczema—swap in codes reflecting those findings.
“The best documentation not only fixes the nails—it covers the whole patient.”
Nailing the clinical diagnosis today sets the stage for precise coding, seamless coverage, and effective treatment. When in doubt, combine your clinical eye with the right lab test and code with confidence—your patients (and your claims department) will thank you.
Documentation Requirements for Accurate Coding and Reimbursement
Essential Elements for Toe Fungus Coding
Every clean claim starts with precise documentation. For toenail fungus, you’ll want to capture a few details in every visit note:
- Diagnosis statement: Use clear terms like “onychomycosis,” “tinea unguium,” or “fungal toenail infection.” Avoid vague impressions like “abnormal nail.”
- Anatomical location: Specify toe vs finger, which foot, and name each affected toenail (example: “right big toenail and third toenail”).
- Number of nails involved: Note if just one, several, or all toenails are affected.
- Laterality: Always state right, left, or bilateral.
- Clinical findings: Describe what you see—color, crumbling, thickening, onycholysis, and subungual debris.
- Pain or complications: Chart any pain, trouble walking, cellulitis, ulcer, or functional impact. These details support the need for treatments like debridement.
If you’ve only made a clinical diagnosis and lab tests are pending, update your codes once results confirm the fungus—that’s how you keep coding accurate, and insurers happy.
A practical visual: Picture a chart with “thick, yellow, brittle right great toenail, pain with shoes, KOH pending”—this level of detail makes billing frictionless.
“When you document with specifics, you’re not just helping your billing office—you’re speeding up patient care and claim approval.”
Capturing Associated Conditions and Risk Factors
Why does charting comorbidities matter? Insurers look closely for risk factors that drive up urgency and cost.
Document all of the following when present:
- Diabetes or neuropathy: Patients with these comorbidities face a greater risk of infection and complications.
- Peripheral arterial disease (PAD): Note for podiatry and diabetic foot care coverage.
- Other risks: Call out secondary conditions like prior ulceration, falls risk, or repeated nail trauma.
- Complications: Chart cellulitis, ulcers, or pain needing intervention—this justifies advanced treatments and supports additional codes like L03.031 or M79.674.
Imagine explaining to a patient: “Writing ‘Diabetic patient with severe nail fungus and ulceration’ helps us get your visits covered.” That’s documentation doing real work.
Avoiding Common Coding Pitfalls
Vague codes put your claims (and your patient’s coverage) at risk. Get specific:
- Never default to unspecified or generic codes—like B49 or B36.9—when chart notes back up onychomycosis or a specific nail involved.
- Update your ICD-10 codes as soon as lab results confirm or change the diagnosis. For example, start with “unspecified” if culture is pending, but switch to B35.1 when onychomycosis is confirmed.
- Don’t forget to code companion conditions when present—like B35.3 for concurrent tinea pedis.
“Details in your notes mean fewer denials and less back-and-forth with the billing team.”
Strong documentation for toe fungus isn’t just best practice—it’s the shortcut to faster reimbursement, fewer denials, and better care. Next time you’re charting, ask: Would my insurance reviewer instantly ‘see’ why this care is necessary? If yes, you’re coding like a pro.
Impact of Toe Fungus ICD-10 Coding on Insurance and Billing
How Coding Influences Coverage and Payment
Every insurance claim for toe fungus starts with the ICD-10 code—and accuracy is everything.
Private and government payers use this code to decide if your diagnosis and treatments are covered, flagged for audit, or outright denied.
B35.1 (Tinea unguium/onychomycosis) signals a documented, billable fungal nail infection. Nail the right code, and your antifungal therapy or nail debridement typically clears approval faster.
But if your claim uses vague, unspecified codes (B35.9 or B49)—or omits supporting details—you’re risking:
- Denied claims requiring rework
- Delays in therapy authorizations
- Higher out-of-pocket costs for the patient
For any antifungal medication, insurance almost always demands proof in the chart—like a “clinical or lab-confirmed diagnosis.” Miss that detail, and you might hit a brick wall.
Quotable tip: “Get specific with your code and your patient’s path to treatment stays smooth.”
Navigating Reimbursement Challenges
Denied claims for toe fungus are often traced right back to coding missteps. Picture this: Your office submits B49 (unspecified mycosis) by mistake. The insurer’s software auto-denies, and now everyone’s chasing paperwork.
Common claim obstacles include:
- Missing laterality or number of nails involved
- Unmatched codes (e.g., treating with nail procedures without supporting B35.1)
- Payers asking for documentation before approving oral antifungals
Move faster by:
- Double-checking chart documentation vs. selected codes before submitting a claim
- Coordinating with your billing team to resolve code mismatches early
- Responding fast to insurance documentation requests to avoid extended denials
Patients rarely see the effort behind the scenes—but you feel it every time a claim pends for weeks.
Quotable scenario: “One code out of place, and that ‘simple’ debridement bill might boomerang back to your inbox.”
Auditing, Compliance, and Future Trends
Audits aren’t just for the big players—random insurance reviews of fungal nail care are rising.
Staying compliant means:
- Using the most specific code possible every time
- Updating codes promptly if lab results come in after billing
- Keeping airtight chart notes that tell the whole story (diagnosis method, extent, treatments, and complications)
Watch for changes: ICD-10 updates hit every October, and digital charting tools (often powered by AI) are increasingly flagging coding errors before claims go out.
Emerging trend: AI-assisted coding is now catching the difference between B35.1 and B49 in real time, helping teams avoid denials and keep compliance sharp.
Quotable stat: “Up to 35% of fungal nail claims are delayed due to incomplete documentation—AI software is out to shrink that number fast.”
Meticulous coding is more than paperwork—it’s the key to unlocking fast, full coverage for your patients and keeping your workflow running like clockwork. When in doubt, code clearly, double-check the supporting chart, and put every diagnosis on the record.
Integrating ICD-10 Coding Into the Broader Toe Fungus Care Journey
Strategic Role in Diagnosis, Treatment, and Prevention
Accurate ICD-10 coding isn't just paperwork—it’s the backbone of quality care from start to finish.
Booking a patient with B35.1 for onychomycosis means the diagnosis, severity, and comorbidities are all documented—creating a roadmap for every step after the visit.
Coding details dictate:
- Which antifungal treatments are approved (topicals, oral meds, or debridement procedures)
- The ability to track response and adjust the plan fast if the infection recurs
- The trigger to escalate care: if labs confirm resistant fungus or if multiple codes show complex infection, it’s your signal to refer to a podiatrist or dermatologist
Picture this: A patient comes in with chronic yellow toenails. Coding both B35.1 and L60.2 (onychogryphosis) instantly flags the case as advanced—payers see the complexity, and the care team knows to monitor for diabetic complications.
Robust documentation makes it crystal clear when prevention steps are needed:
- Counseling for foot hygiene, moisture control, and shoe care
- Setting reminders for rechecks if multiple toenails are at risk
- Recommending lifestyle micro-changes—think “swap out old socks, and let your toes breathe!”
“Every diagnosis code unlocks smarter, safer care—and it’s the first step to making outcomes measurable.”
Connecting Coding Insights to Proactive Care
Granular coding doesn’t stop at today’s visit. It sets you up with historic snapshots, supporting:
- Outcome tracking: Measure how quickly fungal nails clear with topical vs. oral options
- Billing accuracy: Reduce denials for incomplete records and speed up reimbursement
- Quality improvement: Advanced analytics (including AI chart review) can flag patterns, complications, or therapy gaps within your practice
When patients understand these codes on their record, they’re more likely to manage risks and adhere to follow-ups.
Practical tips for next-level engagement:
- Share summaries of the codes used, so patients know what’s documented
- Encourage questions: “Here’s why we used B35.1 for you—it means you can access advanced treatments”
- Invite patients to spot-check their records for accuracy (a win for patient empowerment and compliance)
“Precise codes are more than numbers—they’re your clinical superpower for trend-spotting and future-proofing care.”
Staying current with evolving ICD-10 trends, smart EMR integrations, and proactive documentation isn’t just best practice—it’s what sets high-performing clinics apart.
Key takeaway: Intentional, detailed ICD-10 coding forms the foundation for better toe fungus care, from faster approvals to smarter prevention strategies you can build on year after year.
Conclusion
Mastering ICD-10 coding for toe fungus isn’t just about data entry—it’s your shortcut to smarter billing, faster coverage, and better patient outcomes.
When you choose accuracy and detail, you’re eliminating roadblocks and creating seamless care, both for your clinic and your patients.
Here’s what you can put into action starting now:
- Double down on documentation: Capture the specific nail, laterality, and supporting details for every patient encounter.
- Use precise codes—like B35.1 for confirmed onychomycosis and avoid “unspecified” wherever you can back up your diagnosis.
- Proactively update codes and documentation when lab results return or a patient’s clinical picture evolves.
- Collaborate with your billing team to audit for coding gaps or mismatches before claims go out.
- Keep tabs on insurance policies and leverage AI-powered tools to spot coding errors in real time, reducing denials and rework.
Looking to take the next step?
- Review a recent chart: Could you add more detail or specificity to nail down coverage faster?
- Sync up with your billing and coding team this week to spot opportunities for cleaner claims.
- Try integrating a checklist or smart EMR prompt for companion codes, so nothing slips through the cracks.
Every well-chosen code isn’t just paperwork—it’s a lever for better care, better coverage, and fewer billing headaches. The attention you give to getting it right today will translate into smoother approvals and healthier outcomes tomorrow.
“Precision isn’t extra work—it’s your best shortcut to results.”
Empower yourself and your team to turn every chart, every claim, and every diagnosis into an advantage. When you code with confidence, you lead the way—for your workflow, your practice, and your patients.