Key Takeaways
Untreated toe fungus isn’t just a minor nuisance—it’s a sneaky problem that can spiral into real pain, persistent infections, and even long-term health risks if ignored. Here’s what you need to know (and act on) to protect your feet, your comfort, and your wellbeing.
- Early detection matters—even slight discoloration or brittleness can signal toe fungus, so don’t ignore small changes in your nails.
- Inaction leads to escalation: Fungus thrives over time, causing thickened, misshapen nails that can make walking painful and shoes unbearable.
- Fungus is a team player: It spreads easily to other nails, skin, and even household surfaces—sharing socks or grooming tools is a fast way to spread infection.
- Complications get serious fast: Ignoring infections can invite bacteria, causing severe issues like cellulitis, abscesses, or even bone infection—not just a cosmetic concern.
- Chronic infection means permanent damage: Long-term toe fungus can cause irreversible nail changes, painful ulcers, or nail loss that may require surgery.
- At-risk groups face higher stakes: If you have diabetes, weak immunity, or poor circulation, untreated fungus can escalate from mild discomfort to dangerous infections or wounds.
- Treatment is your power move: Act early with topical or prescription therapies—catching fungus early means less pain, less cost, and higher odds of a full recovery.
- Daily prevention keeps fungus away: Keep feet dry, don’t share personal items, and sanitize grooming tools to protect yourself and others from a stubborn, recurring issue.
Don’t let a minor nail change become a major headache—catching and treating toe fungus early is the quickest way to keep your steps easy, pain-free, and infection-free. Dive into the full article for smart prevention strategies and actionable treatment options!
Introduction
You glance down and spot a faint yellow patch on your big toe. Annoying? Sure. Urgent? Not so much—right? Here’s the kicker: up to 14% of adults walk around with a hidden fungal nail infection, often ignoring it until things get downright unpleasant.
For many tech-savvy professionals, a small cosmetic issue quietly snowballs—affecting not just you, but your family, your gym, and even your day-to-day mindset. What’s “just a minor spot” today could morph into months of soreness, lost time, or even serious medical complications if left unchecked.
The reality? Untreated toe fungus rarely stays put. Left alone, it can:
- Silently spread to other toes, your skin, and anyone sharing grooming tools
- Trigger pain, thickening, or actual nail loss—making simple tasks awkward or painful
- Open doors for persistent infections that transform a quick fix into a long-term frustration
Think of foot fungus like that neglected app update—ignore it, and the glitches eventually spiral into more headaches (and possibly expensive repairs).
Here's what you’ll gain from this read:
- Spot crucial early warning signs (so you can act before it spirals)
- Discover real-world risks beyond “ugly nails”—from infection to chronic pain
- Get actionable habits and prevention tips that fit into your workflow—because foot problems shouldn’t side-track your busy day
If you’ve ever brushed off a “harmless” nail change, you’re not alone—but you do have the power to stop the domino effect before it starts.
So, what actually happens when you press pause on treatment? Let’s walk through how toe fungus takes hold, why every month matters, and how catching trouble early saves you more than a little embarrassment.
How Untreated Toe Fungus Progresses
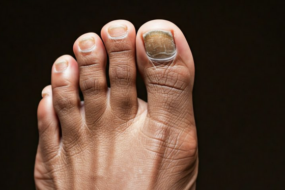
Picture this: toe fungus starts off nearly invisible, a tiny change beneath the surface of your nail. Most people notice a faint yellow spot or some mild discoloration, but—like a weed quietly sprouting under the soil—it rarely screams for your attention at first.
Recognizing Early and Moderate Stages
In the beginning, here’s what to watch for:
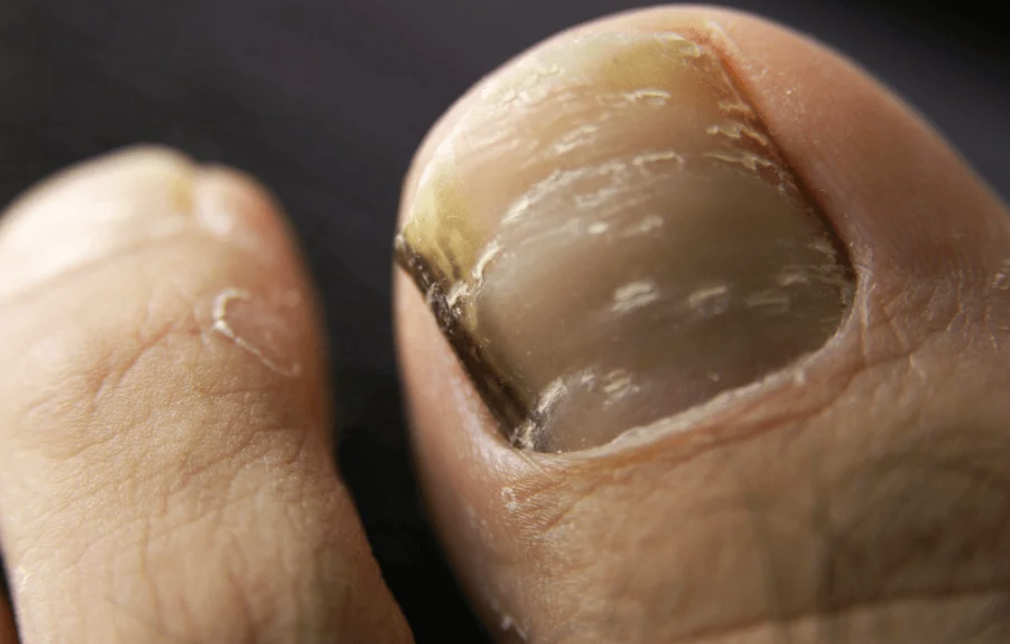
- Slight nail discoloration: pale yellow, white, or brown spots
- Mild thickening or brittleness: the nail feels more dense or crumbly
- Rough surface texture and subtle dullness
Often, these changes get brushed off as “just aging” or a stubbed toe. It’s easy to miss the signs until the problem literally grows.
How the Fungus Advances
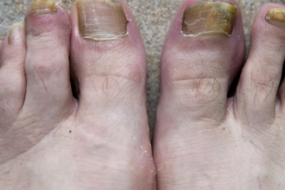
Over months (sometimes years), fungus burrows deeper into the nail and beyond the nail bed. If left alone, you may see:
- Significant thickening making it tough to trim the nail
- Distortion: nail warping, lifting, or even separating from the skin
- Crumbling or breaking at the edges
This isn’t just about looks. A thick, misshapen nail makes wearing shoes uncomfortable—or even walking painful.
Beyond the Nail: Slow, Sneaky Progression
What’s wild? Many people don’t feel real pain until nail deformity or secondary infections take hold. Picture an athlete who ignores “just a small spot” only to find, a year later, they can’t run without limping.
Here’s what often happens:
- Fungus sneaks into new territory: infects other toes, spreads to the skin (hello, athlete’s foot)
- Stable damage sets in: advanced cases can leave the nail permanently thickened or even cause lasting deformity
- Silent progression: the fungus grows more resilient with time, making future treatments longer and tougher
“Think of ignoring toenail fungus like letting a leak drip under your kitchen floor—the longer it runs, the bigger the mess you’ll have to fix.”
Key Takeaways You Can Use Right Now
- Spotting early changes is critical: even tiny color or texture shifts matter
- Don’t wait for pain—by the time your toe hurts, nail damage may be severe
- Every month counts: what starts as a “cosmetic” issue can become a true medical problem over time
Catching toe fungus early is like fixing a small pothole before it ruins your tires. The sooner you act, the less damage you’ll face—and the easier it is to reverse.
Immediate and Progressive Risks
Spread of Fungal Infection
A single case of untreated toe fungus isn’t just your problem—it’s a risk to everyone around you.
Fungal spores are surprisingly persistent and can migrate far beyond one nail. You might notice the infection spreading:
- To other toenails or fingernails—think of it as a “domino effect” on your feet and hands.
- Onto the surrounding skin (where it commonly triggers athlete’s foot).
- All the way to the genitals, causing jock itch in rare but real scenarios.
- On household surfaces—floors, showers, and even inside shoes—for days.
Picture this: You clip your infected toenail and use the same cutter on your hands. Next thing you know, “that stubborn yellow patch” jumps ship to your fingernail—yikes!
How Fungal Infections Travel
You’re not immune just because you don’t share shoes—everyday items can be silent transmitters.
Watch out for:
- Shared grooming tools—clippers, nail files, pumice stones
- Towels, socks, gym mats, or communal showers
- Footwear swaps or keeping shoes on warm, damp surfaces
- Close contact with family, roommates, or gym members
If you’re a parent, consider this: Kids can easily bring these spores to school locker rooms, spreading it without a clue.
Pain, Discomfort, and Daily Impact
Ignoring toe fungus doesn’t make it go away—instead, you’ll likely face a cascade of physical hassles.
Misshapen or thickened nails start to hurt. Over weeks to months, you may notice:
- Constant soreness or pressure with every step
- Trouble running, walking, or wearing closed shoes comfortably
- Ingrown nails that dig painfully into surrounding skin
- Stubbed toes that bleed or rip, thanks to brittle, warped nails
On busy days, even slipping on your favorite sneakers can feel like a chore. One jog could go from workout to work injury if you’re unlucky.
Actionable Takeaways
- Don’t share grooming tools or shoes to curb household spread.
- Catch symptoms early—thickening, discoloration, or itching should spark instant action.
- Treat foot hygiene as a team sport—especially in shared spaces like gyms or homes.
The longer you ignore toe fungus, the wider it spreads and the harder it is to control. Acting now is the best way to save yourself—and everyone you care about—from a fungal domino effect.
Complications Beyond the Nails
Secondary Bacterial Infections
When toe fungus cracks or splits your nail, it’s like leaving your front door wide open to trouble.
Once the protective nail barrier is broken, bacteria can easily sneak in, causing problems beyond the surface.
Picture this: You notice your toe is suddenly red, swollen, hot, and really tender—those are classic signs of cellulitis, a serious skin infection that needs urgent medical attention.
If left unchecked, things get heavy fast. Severe outcomes can include:
- Abscesses (painful pus-filled pockets under the skin)
- Tissue breakdown, where the skin and flesh literally start to deteriorate
- Rare but critical dangers like sepsis (bodywide infection), osteomyelitis (bone infection), or even gangrene (tissue death)
One vivid scenario: A simple split toenail develops a painful, throbbing infection that spreads up the foot—the difference between a quick clinic visit and weeks in the hospital often comes down to early action.
“A cracked toenail can open the door to infections that land you in the ER.”
“What starts as a minor split can spiral into tissue damage or bone infection if ignored.”
Permanent Nail and Tissue Damage
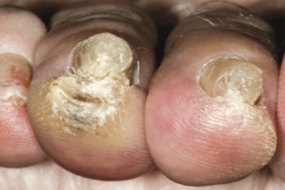
When fungus sticks around for months or years, it starts leaving permanent footprints.
Chronic onychomycosis (the medical term for long-term fungal infection) leads to:
- Thickened nail beds that feel like tough, yellow armor
- Permanent ridging and changes in nail shape
- Hyperkeratosis (hard, crusty buildup beneath the nail)
- Ulceration or open sores that just won’t heal
For some people, especially if treatment is delayed, the nail never regrows healthy—even if the fungus finally dies.
In these cases, you may face:
- Surgical nail removal, which is exactly as intense as it sounds
- Difficulty (or impossibility) of the nail ever regrowing properly
- Sometimes, permanent nail loss and ongoing pain when wearing shoes
Imagine seeing a toenail crumble away or become so thick and distorted you have to cut it in layers—a scenario many ignore until daily life is affected.
“Letting toe fungus linger can leave permanent scars—sometimes the nail never comes back.”
“Every year you wait, you raise the odds you’ll need surgery or never see a healthy nail again.”
If unchecked, toe fungus isn’t just a cosmetic issue; serious infections and irreversible damage can follow.
The takeaway: The longer toe fungus goes untreated, the higher the stakes—early action is always your safest bet.
Long-Term and Systemic Effects
Recurrent and Systemic Spread
Untreated toe fungus isn't just a nuisance—it’s a master of hiding and recurring. Picture spending years battling brittle, yellow nails, only to have them clear up and boomerang back.
Studies show recurrence rates range from 5% to 50%, even after aggressive treatment. That’s a coin toss between clear nails and another round of discomfort.
Fungus doesn’t like to stay put, either. In rare cases, especially for those with other health challenges, these invaders can travel from the nail bed deeper into surrounding tissue—or, alarmingly, the bloodstream.
Real talk: leaving toe fungus untreated can open doors to chronic infection, tissue breakdown, and a cycle that feels impossible to break.
What does this look like day-to-day?
- Persistent nail thickening, discoloration, and decay, sometimes for years
- Frustrating “clear up—relapse” cycles, even when you follow treatment plans
- Growing risk for deep fungal invasion if ignored, especially if you’re managing another illness
“Think of untreated toe fungus as that one persistent pop-up ad—ignore it, and it keeps coming back bigger each time.”
Amplified Risks for Vulnerable Groups
Certain medical conditions can turn toe fungus from pesky to dangerous in a hurry. If you have diabetes, weakened immunity, or poor circulation, the stakes go up fast.
Here’s why these groups face more serious complications:
- Higher risk of severe infections like cellulitis or bone infection
- Small cracks from fungus can trigger massive health issues
- Faster progression—what might be slow in a healthy adult can escalate to hospitalization in weeks for someone with diabetes or vascular disease
Imagine a senior's mild toenail fungus quietly turning into a chronic wound or, worse, amputation. It’s not just a scare story—up to 20% of serious diabetic foot infections start as simple nail fungus.
“Even a mild, ignored toe fungus can be the domino that tips over a whole row of health complications.”
Takeaway
If you or someone you know fits into these risk groups, don’t hit snooze on early treatment. Persistent or recurring nail fungus carries risks that reach far beyond appearance—especially for those managing chronic health conditions. A smart, fast response is always the best move.
Why Early Treatment Matters
Preventing Escalation and Long-Term Damage
Ignoring toe fungus isn’t just a cosmetic issue—it’s an open invitation for big problems down the line.
Early treatment stops the “slow motion domino effect” where mild symptoms become chronic, painful, and even permanent.
With prompt care—whether it’s:
- Topical antifungals you apply at home
- Prescription pills or laser treatments from your doctor
- Surgical nail removal for severe damage
—you can block serious progression and avoid the harshest complications.
Nail growth is frustratingly slow (think millimeters per month), so patience is a must.
Most people see visible improvement in 6–12 months, but some nails take up to a year to fully grow out clear.
Skipping treatment lets fungus burrow deeper, making full recovery much less likely—kind of like letting weeds take over your lawn for a whole season.
Worried about cost, embarrassment, or not knowing if it’s fungus?
Podiatrists and dermatologists guide you with fast, accurate diagnosis and custom solutions, so you don’t waste time (or money) guessing at the drugstore.
Real-World Outcomes and Prevention
Picture this: One person with untreated fungus passes spores to their family using the same nail clippers.
A year later, three people are dealing with messed-up nails and itching.
Meanwhile, someone who tackled it early avoided this entire chain reaction—and kept their sandals in play for summer.
To protect yourself and others:
- Keep feet clean and dry
- Disinfect or replace grooming tools regularly
- Never share socks, shoes, or towels
- Treat athlete’s foot immediately—don’t give fungus a shortcut
Remember, recurrence happens in 5–50% of cases after treatment if infections go ignored or hygiene slips.
“A little action now beats a lot of regret later”—your future self, and your feet, will thank you.
Early intervention isn’t just about better-looking nails; it means less pain, fewer doctor visits, and lower risk for your whole household.
Taking that first step today is the ultimate power move—especially when you know the alternative is months (or years) of stubborn, spreading problems.
Conclusion
Taking toe fungus seriously means breaking the cycle before it spirals into pain, discomfort, and even health risks for your whole household.
Every day you wait gives fungus more ground to cover and makes recovery that much harder.
Staying proactive is your ticket to healthier feet, fewer complications, and more freedom—whether that means running a marathon or just enjoying open-toed shoes with confidence.
Here’s what will set you up for the best results:
- Act on early symptoms—don’t let minor discoloration or thickening slide.
- Disinfect all grooming tools after every use, especially if you share your space.
- Treat athlete’s foot fast to head off future infections, both on your feet and beyond.
- Avoid sharing towels, socks, or shoes to minimize household transmission.
- Ask a podiatrist or dermatologist for guidance if you’re unsure or symptoms progress.
Now, don’t just file this info away—take 10 minutes today to inspect your nails, clean your tools, and set a reminder on your phone for a weekly check-in.
If something looks off, make that call or pick up a proven fungal treatment—because the fastest wins come from early action.
Healthy feet aren’t just a cosmetic bonus—they’re your foundation.
Choose action today and future-you will thank you for every confident step you take.
“Prevent big problems by acting on the small ones—your toes, your health, and your peace of mind will all catch the benefits.”