Key Takeaways
Understanding sleep apnea doesn’t have to be complicated—you just need the right insights at your fingertips. Here’s what tech-savvy professionals need to know to spot, tackle, and manage sleep apnea like a pro—whether you’re optimizing your health or just trying to make those mornings count.
- Sleep apnea is an invisible sleep disruptor that causes your airway to repeatedly block or collapse, leading to fragmented rest and serious drops in blood oxygen.
- Obstructive Sleep Apnea (OSA) dominates the landscape, making up 84% of adult cases, and is most common in men aged 40–70, but can affect anyone—including younger adults and post-menopausal women.
- Key warning signs include loud snoring, gasping, and crushing daytime fatigue—if you (or your smartwatch) notice persistent tiredness despite enough hours in bed, start asking questions.
- Untreated sleep apnea dramatically increases risk for high blood pressure, heart attack, stroke (up to 3x risk), and type 2 diabetes, while also tripling your odds of car accidents due to daytime sleepiness.
- Diagnosis is smarter than ever, using tools like STOP-BANG and home sleep apnea tests (HSAT) for straightforward cases, with full in-lab polysomnography (PSG) for deeper insights when symptoms are unclear.
- Treatment is highly personalized—no “one size fits all” approach, with effective options like CPAP therapy (cutting cardiac risks by nearly 50%), oral appliances, nerve implants, surgery, and even simple lifestyle tweaks.
- Tech upgrades and habit stacking simplify daily life with sleep apnea: use smart apps, travel-friendly devices, and environmental changes (like blackout curtains) to embed therapy into your routine.
- Open conversations with your doctor and partner help catch issues early—logging symptoms and feedback leads to faster solutions and more restful nights.
Learning to recognize and manage sleep apnea is a game-changer for your health and productivity—dive into the main article to get expert strategies, practical tech tips, and actionable solutions you can start using tonight.
Introduction
It’s hard to believe, but up to 1 in 5 adults suffers from a hidden culprit that can torpedo productivity, mood, and even heart health—most without realizing it’s there.
Have you ever crushed a full night’s sleep, checked your stats, and still felt like a zombie by noon? That “sleep debt” might not just be about stress or screen time—it could be sleep apnea disrupting your brain and body, night after night.
Here’s the wild part: sleep apnea doesn’t care if you’re tech-savvy or health-conscious. Instead, it quietly rewrites everything from your focus at work to your risk of stroke, all under the radar. For the high-achievers and problem-solvers in the room, just imagine how sustained low oxygen and sleep fragmentation can steal sharp thinking, creativity, and the mental edge that fuels your work.
Curious if you should care? If you—or your smartwatch—track signs like:
- Daily drowsiness, despite “enough” sleep
- Productivity dips after lunch that coffee can’t fix
- A partner complaining about sudden snoring or gasping
…then this is a conversation you can’t ignore.
In the next few minutes, you’ll get:
- A clear, scan-friendly breakdown of what sleep apnea really is (spoiler: it’s much more than “just snoring”)
- The latest on hidden health risks (and exactly why leaving symptoms unchecked can spell trouble for body and brain)
- Modern diagnosis tech and pragmatic solutions—from streamlined home sleep tests to lifestyle tweaks and smart devices that actually fit your workflow
You’ll also see surprising patterns and stories that help connect the dots—whether you geek out on data or just want sharper mornings.
If better nights and clearer days sound appealing (and who doesn’t want an extra gear?), keep reading. Understanding sleep apnea is the first, crucial step toward taking back your energy—and your edge.
Ready to see what’s really happening when you sleep? Here’s what you need to know about sleep apnea, who gets it, and how it quietly sabotages your best efforts.
What Is Sleep Apnea? Core Concepts and Types
Sleep apnea is when your breathing repeatedly stops and starts during sleep, causing fragmented rest and unhealthy drops in blood oxygen.
Imagine your airway as a flexible tube—during sleep, it can collapse, narrow, or become blocked, making airflow grind to a halt.
Your brain jolts you awake just enough to reopen the airway, even if you never fully realize it. The result: constant cycles of disruption, poor-quality sleep, and a body left begging for rest.
The Three Main Types—Visualized
- Obstructive Sleep Apnea (OSA): Physical blockage of the airway—think of it like a kinked garden hose that stops water (air) from flowing.
- Central Sleep Apnea (CSA): The brain fails to send proper breathing signals, so no effort is made to inhale.
- Complex/Mixed Sleep Apnea: A blend where both blockage and brain signaling issues play a role—like a traffic jam with stalled cars and a faulty traffic light.
About 84% of adult cases are OSA, making it far more common than the other types.
Who Gets Sleep Apnea? Patterns, Prevalence, and Triggers
Sleep apnea doesn’t have a “type.” It affects people across every age and gender, but some groups are more at risk:
- Men aged 40-70 (but women post-menopause catch up fast)
- People with obesity or a large neck circumference (≥ 17 inches for men, 16 for women)
- Anyone with a family history or certain anatomical differences (like a recessed jaw)
- Frequent alcohol use, smoking, or using sedative medications
Roughly 1 in 5 adults has at least mild sleep apnea, though most remain undiagnosed.
Warning Signs: What You—and Your Partner—Will Notice
Watch for these everyday red flags:
- Loud, habitual snoring
- Sudden waking or gasping for air
- Chronic, unrefreshing sleep or morning headaches
- Your partner says you stop breathing or choke in your sleep
- Daytime fog, trouble concentrating, or that nap-you-can’t-resist feeling
A relatable scenario: Picture this—your afternoon productivity tanks, coffee does nothing, and your smartwatch shows you’re sleeping eight hours but still exhausted. Could it actually be sleep apnea?
Key Takeaways
Sleep apnea is more than just snoring—it’s an invisible cycle that silently sabotages your health.
Recognizing the warning signs and risk factors puts you in control to seek help, protect your long-term wellbeing, and finally reclaim your energy.
“If you feel like sleep just isn’t working for you, it’s time to start asking questions—your body will thank you.”
Health Risks and Consequences of Untreated Sleep Apnea
If you think sleep apnea is just about snoring, think again—this condition can quietly trigger a storm of health threats that touch nearly every system in your body.
Repeated oxygen drops during the night cause “fight or flight” hormones to surge, wear out blood vessels, and disrupt your metabolism.
Not Just Sleepy: Major Body-Wide Complications
Untreated sleep apnea is linked to dramatic cardiovascular dangers, including:
- Hypertension (high blood pressure)
- Atrial fibrillation (irregular heartbeat)
- Heart attack and heart failure
- Stroke (with men facing a threefold risk increase)
Picture this: Every pause in breathing acts like a micro-stress test for your heart, all night long.
Metabolic and Brain Health at Risk
The damage isn’t just to your heart.
Sleep apnea kicks up your risk for:
- Type 2 diabetes and worsened metabolic syndrome
- Acid reflux and liver problems
Cognitively, you might notice:
- Memory lapses
- More depression or anxiety
- Brain fog (even a higher risk of “silent” brain damage over time)
Daytime fatigue can be brutal, leading to mistakes at work, falling asleep during meetings, or—most dangerously—drowsy driving. In fact, people with untreated OSA have triple the risk of traffic accidents.
Surgery and Hospital Risk Factor
Heading in for surgery? Hospitals now flag undiagnosed OSA as a major surgical risk because:
- It raises the odds of cardiac arrest
- Increases the chance you’ll need ICU care
- Ups the likelihood of serious breathing complications
Visual Snapshot: Warning Flags
If you notice two or more of these, consider a sleep study:
- Loud, persistent snoring
- Sudden nighttime gasping or choking
- Unexplained morning headaches
- Crushing fatigue, especially in the afternoons
- Mood changes (irritability or depression)
- Loss of focus or frequent memory slips
Severity Multiplies Risk
The rule is simple: The more severe your sleep apnea, the greater your risk of dangerous outcomes.
Ignoring the problem won’t make it go away—left untreated, sleep apnea becomes a silent driver of chronic illness and life-altering accidents. Recognizing the warning signs is step one; getting an assessment is your fast track to protecting your heart, brain, and safety.
How Sleep Apnea Is Diagnosed: Processes and Technologies
Recognizing sleep apnea isn’t always straightforward—even for experts.
Daytime sleepiness, concentration lapses, and snoring often blend in with “normal” life or get blamed on stress.
The Diagnostic Journey Starts With Questions
Your doctor will likely begin with screening tools to spot risk factors quickly.
The most popular?
- STOP-BANG: Eight powerhouse questions covering snoring, tiredness, high blood pressure, BMI, neck size, age, and more
- Epworth Sleepiness Scale: Measures how likely you are to doze off, even during zoom calls or in waiting rooms
If you score high, it’s go-time for a sleep study—because “normal” tiredness could actually be apnea in disguise.
Breaking Down the Gold Standard: Polysomnography (PSG)
PSG is the gold standard—think of it as a full night’s “sleepscape” recorded in a lab.
What’s measured?
- EEG (brain waves) to track sleep stages
- EKG (heart rhythm) for cardiovascular clues
- Airflow, oxygen, movement sensors to catch every pause, gasp, or leg twitch
Picture this: You’re tucked into a quiet room, sensors comfortably placed, while a team observes your every snore and sigh—no guesswork here.
Fun fact: A split-night PSG may switch you onto CPAP therapy halfway if doctors spot problems fast.
Not everyone needs the full in-lab experience.
Home Testing or In-Lab? Choosing the Right Fit
For suspected uncomplicated obstructive sleep apnea, a Home Sleep Apnea Test (HSAT) is often enough.
HSAT measures:
- Airflow
- Oxygen levels
- Heart rate
But it’s less detailed—no brain wave tracking. If you have heart, lung issues, or unclear symptoms, you’ll still need PSG for answers.
Understanding Results: The Apnea-Hypopnea Index (AHI)
After testing, doctors calculate your AHI—the number of breathing issues per hour.
Severity breakdown:
- Mild: 5–15
- Moderate: 15–30
- Severe: 30+ events/hour
A quick takeaway: The higher your AHI, the greater your health risks—so numbers really matter.
When to See a Specialist and What It Means For You
Don’t wait for symptoms to snowball.
- See a sleep specialist if you:
- Wake up gasping
- Snore loudly
- Face daily fatigue
Early diagnosis means you can reclaim lost energy—the sooner you know, the sooner you change your life.
Key takeaway: “Diagnostic clarity is step one. If you’re tired of guessing, these tools put answers (and energy) within reach.”
Modern Treatment Strategies for Sleep Apnea
Finding the Right Fit: No “One Size Fits All” in Sleep Apnea Care
Effective treatment is absolutely possible—and for many, it’s life-changing.
But here’s the catch: what works wonders for one person may frustrate another. Sleep apnea therapies are all about custom solutions and comfort.
CPAP Therapy: First-Line, Highly Effective—But Not Always Easy
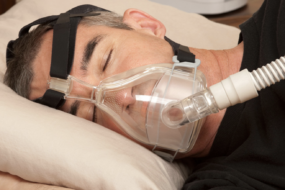
CPAP (Continuous Positive Airway Pressure) uses a gentle, steady stream of air via a mask while you sleep.
- Gold-standard for moderate and severe OSA
- Works by preventing airway collapse—think of it as a “nightly air splint”
- Dramatically drops risk of heart attack and stroke by nearly 50%
That said, up to 50% of users ditch CPAP early due to:
- Discomfort from the mask or air pressure
- Trouble traveling with bulky equipment
- “CPAP face”—awkward straps, dry mouth, or leaky seals
If you’re wrestling with CPAP, try:
- Mask fitters or heated tubing for better comfort
- Humidifiers to reduce dryness
- Apps and smart machines that track and optimize your progress
“Picture this: A well-fitted CPAP rig becomes nearly invisible in your nightly routine—like your favorite pair of sneakers, but for sleep.”
Other Treatments: Bite Guards, Implants, Surgery, and Lifestyle Tweaks
Options abound for those who can’t stick with CPAP or have mild cases.
- Oral Appliances (“bite guards”): Useful for jaw or tongue blockade. Pros: portable, quiet. Cons: less effective for severe apnea, can cause tooth movement.
- Hypoglossal Nerve Stimulation (HNS): An implant (about the size of a pacemaker) that “nudges” your tongue forward at night. 11% report side effects like tongue abrasion—but for the right person, it’s a tech-forward fix.
- Surgery: Considered for very specific anatomical issues or severe, CPAP-resistant apnea. Procedures can range from tonsil removal to complex skeletal adjustments—each with its own risk/reward profile.
- Lifestyle Changes: Weight loss, exercise, sleeping on your side, and skipping sedatives/alcohol can make a measurable difference.
“Think of sleep apnea care like picking running shoes: custom fit means better results, whether you need sneakers or orthotics.”
The Power of Personalization—and When to Take Action
Partnering with a sleep specialist dramatically boosts your odds of long-term success. You get:
- A tailored game plan for your unique anatomy, risk factors, and lifestyle goals
- Ongoing tweaks to keep you motivated and sleeping better
Remember, sticking with therapy can drop cardiac risks by 50% and transform energy, focus, and mood.
If you’re tired of waking up exhausted, your go-forward playbook starts with an honest talk with a sleep pro—the right strategy means “good nights” can finally become your norm.
Living with Sleep Apnea: Practical Tips and Real-World Strategies
Managing sleep apnea day-to-day isn’t just about plugging in a CPAP and hoping for the best.
You’ll want smart routines and simple tweaks that fit your actual lifestyle—think habit stacking for healthy sleep.
Here’s what can make an instant difference:
- Set a consistent bedtime (even on weekends) to anchor your sleep schedule.
- Use blackout curtains, a cooling pillow, or white noise to optimize your sleep environment.
- Keep your CPAP gear clean and ready—think “toothbrush for your mask” each night.
Quotable: “Good sleep isn’t just a goal, it’s your real competitive edge—especially with sleep apnea in the mix.”
Communication and Support: Talking to Your Doctor and Partner
Sleep apnea thrive when ignored, but gets manageable when you open up.
Here’s how to keep the right conversations flowing:
- Share symptoms and concerns with your doctor—log your sleepiness, morning headaches, or device struggles.
- Ask for solutions, not sympathy: “What adjustments could help my device fit better?” can save months of frustration.
- Invite your partner into the loop, so they can spot warning signs like loud snoring or night awakenings you might miss.
Even a two-minute check-in can change your care pathway.
Tech Tools, Travel Tips, and Real Lifestyle Solutions
Managing sleep apnea gets easier (and sometimes cooler) with tech.
Try:
- Sleep-tracking apps or smartwatches that flag nights with poor oxygen or excessive movement.
- Compact travel CPAPs—yes, they exist and fit in a carry-on.
- Pre-set alarms to remind you to use your device during hectic shifts or travel.
Quotable: “Most sleep tech is only as helpful as the habits you build around it—stacking smart with simple works best.”
Busted Myths, Motivation, and the Sleep Apnea Community
Let’s clear up some myths: sleep apnea isn’t just for “heavyset men over 50”—it can hit anyone.
Here’s what keeps you thriving:
- Don’t skip treatment, even if you feel “fine”—untreated OSA triples stroke risk.
- Join online sleep support groups, or follow sleep health pros to stay motivated.
- Experiment: remix your routine and share what works—your tweaks might inspire others.
Picture this: Recharging after just one week of proper sleep apnea therapy—less brain fog, fewer mistakes at work, and maybe even a little extra patience in your day.
Taking small steps every day makes the entire journey less overwhelming.
Remember: building a custom sleep routine, staying vocal with your care team, and leveraging tech gives you real control—restorative sleep is a skill, not just an outcome.
Conclusion
Understanding sleep apnea isn’t just about identifying a sleep problem—it’s about taking back your daily energy, protecting your health, and setting yourself up for genuinely restorative rest.
Every step forward brings you closer to better focus, sharper thinking, and a body that works with you—not against you. Knowledge only has power when you put it into action.
Key Takeaways for Real Impact:
- Prioritize a sleep assessment if you recognize warning signs like loud snoring, morning fog, or gasping at night.
- Embrace the right treatment for you—whether it’s CPAP, an oral appliance, lifestyle adjustments, or cutting-edge therapy.
- Stack healthy sleep routines: keep a consistent bedtime, optimize your bedroom, and treat your device maintenance like any essential daily habit.
- Leverage tech tools—from smart trackers to travel-ready masks, let digital solutions boost your consistency and insight.
- Create a support system: keep the conversation open with your doctor and your partner; shared vigilance leads to lasting results.
Next Steps You Can Take Today:
- Start a sleep journal or log using your phone—record symptoms, wake-ups, and how you feel each morning for the next week.
- Schedule a consult with your healthcare provider—advocating for yourself is the first move toward better sleep and brighter days.
- Try one environmental or tech tweak tonight, like blackout curtains or a sleep-tracking app, to see immediate little wins.
- Share one key takeaway from this guide with a friend, partner, or colleague—amplifying awareness helps everyone around you.
Getting your nights right means your days get better—sleep isn’t a luxury, it’s your everyday launchpad for health, focus, and true vitality.
You have the tools and knowledge. Now’s the time to make restorative sleep your competitive advantage—because a rested mind is unstoppable.