Key Takeaways
Confusing cellulite with cellulitis is more common than you’d think—and knowing the difference can save you time, stress, and even a trip to the ER. Here’s a quick-hit guide to help you confidently spot, assess, and respond to each condition with zero guesswork.
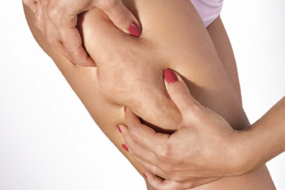
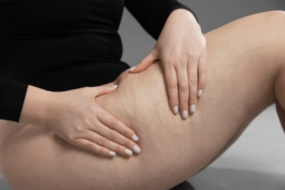
- Cellulite is cosmetic and harmless—it appears as lumpy, “orange peel” skin, especially on thighs and hips, and affects up to 90% of women with no health risks.
- Cellulitis signals a serious infection—look for sudden redness, heat, swelling, and pain that often spreads rapidly and may come with fever or feeling unwell.
- Appearance is the first clue—cellulite looks like dimples with no redness or warmth, while cellulitis shows red, hot, and glossy patches that change fast.
- Risk factors differ completely—cellulite runs in families and is driven by genetics and hormones, while cellulitis strikes through breaks in the skin, especially in people with diabetes or immune issues.
- Treatment urgency matters—cellulite management is optional and cosmetic, but cellulitis demands immediate antibiotics and medical attention to prevent serious complications.
- Self-diagnosis has real risks—mistaking cellulitis for cellulite can delay life-saving care; don’t rely on photos alone—trust your symptoms and act quickly if you see redness spreading or feel ill.
- Simple rule of thumb: “No pain, no fever, likely cellulite. Red, hot, and sick? Doctor time.”
- Knowing the difference protects your health—spot changes early, trust your gut, and when in doubt, always err on the side of urgent care.
When you’re scanning your skin, these essentials will help you avoid confusion, seek help when needed, and skip the WebMD rabbit hole. Want deeper guidance or a symptom checklist? Dive into the full article for expert insights.
Introduction
Ever googled a skin issue and been alarmed by how similar “cellulite” and “cellulitis” sound—only to realize one’s a harmless cosmetic quirk and the other could land you in the ER?
You’re not alone. Nearly 90% of women experience cellulite at some point, but misunderstanding these two terms can cause unnecessary panic—or, worse, dangerous delays in treatment.
For tech-savvy professionals like you, accuracy matters. Distinguishing between these conditions isn’t just about looking good on camera or feeling comfortable in your jeans. It's about protecting your health and making confident, informed decisions when it counts.
Let’s clear up the confusion in minutes, not hours lost on Reddit or WebMD rabbit holes.
Here’s what you’ll walk away with:
- Crystal-clear definitions: No jargon or medicalese—just simple visuals, relatable examples, and a direct “is this urgent?” litmus test
- A quick-scan breakdown: The most obvious signs, risk factors, and red flags—so you can spot the difference instantly
- Key takeaways for action: Know when to relax, when to call your doctor, and how to communicate clearly if you need help
Think of this as your practical toolkit: you’ll leave knowing exactly what’s safe to ignore, what’s worth a tweak in your routine, and what’s an instant doctor call—without getting lost in technical language or scare tactics.
Ready to trade stress for clarity? Up next: how a dimpled thigh and a red-hot leg aren’t even close—here’s how to recognize the real difference, fast.
Understanding Cellulite and Cellulitis: Definitions and Core Differences
Cellulite and cellulitis: same-sounding, worlds apart. If you've ever wondered why these terms get mixed up, you're not alone—cellulite is a cosmetic issue, while cellulitis is a medical emergency.
Cellulite is what gives skin that dimpled, “orange peel” look—think of the soft rippling on a cushion. It's all about the way fat and connective tissue interact just beneath your skin’s surface, most often on your thighs, buttocks, and hips.
What Each Condition Really Means
- Cellulite
- Cosmetic: visible “dimples” or lumpiness under the skin
- Not harmful: doesn’t signal infection or cause illness
- Super common: up to 90% of women experience it at some point
- Cellulitis
- Serious Infection: caused by bacteria (usually strep or staph) invading deeper layers of the skin
- Red, hot, swollen, and painful: often with fever and spreading rapidly
- Risks: Can affect anyone but more dangerous for those with diabetes, obesity, poor circulation, or weakened immune systems
Picture this: Cellulite is dimples in a mattress—visible but harmless. Cellulitis is a sudden, red-hot patch like a warning flare on your skin.
Why These Names Create Confusion
It’s easy to see why these terms get tangled:
- Both involve changes in the skin’s appearance
- The names sound nearly identical
- Google results can be misleading if you’re not sure what to look for
But here’s the cliff note: Cellulite doesn’t need the ER; cellulitis might.
Quick-Reference Table
If you’re staring at a mystery patch of skin, ask yourself: “Is it just bumpy, or is it getting red, hot, and spreading?” If it’s the latter, see a doctor—fast. The key takeaway: knowing the difference protects your health and stops confusion at the source.
Causes and Risk Factors: What Leads to Each Condition?
Cellulite: Under-the-Skin Structure and Influencing Factors
Cellulite isn’t about infection or hygiene—it’s a quirk of your body’s anatomy.
Picture this: beneath your skin, fat cells are pushed up against the skin while fibrous bands pull the skin down, creating that dimpled, “orange peel” look.
This occurs most often in areas with more natural fat padding—think thighs, hips, buttocks, and sometimes the abdomen.
The drivers behind cellulite aren’t about what you do, but who you are. Here’s what influences it:
- Genetics: If your family has cellulite, your odds go up.
- Hormones: Especially estrogen—one big reason about 90% of adult women see cellulite at some point (guys, you’re far less likely).
- Aging: Skin gets thinner and connective tissue bands tighten as you get older.
- Weight changes: Gaining or losing weight can make cellulite more visible or pronounced.
- Body fat distribution: Some people naturally store fat in cellulite-prone areas.
For example, a busy professional who sits most of the day may notice more dimpling over time—not because they’re unclean, but because structure matters more than surface.
Myth alert: Cellulite is absolutely not a sign of poor hygiene or an infection.
Cellulitis: How Infections Take Hold
On the flip side, cellulitis is a red-alert for infection.
This condition happens when bacteria (mainly strep or staph) sneak through skin breaks—tiny or big—like:
- Scrapes, cuts, or insect bites
- Cracked skin (think dry feet, eczema, athlete’s foot)
- Surgical wounds or ulcers
Certain groups face higher risk:
- People with diabetes, obesity, or poor circulation
- Those with a weakened immune system (from illness or medications)
- Anyone with lymphedema, a history of cellulitis, or limited mobility
- Injection drug users
Imagine you’re gardening and scrape your leg. What starts as a mild irritation could, if left untreated, evolve into an expanding, hot, red patch—that’s cellulitis moving in.
Ignore cellulitis at your own risk: it’s fast, can lead to fever, and might even send you to the ER.
Key Visualizations and Takeaways
- Cellulite = long-term skin dimpling, almost always harmless.
- Cellulitis = sudden, red, painful swelling—always take seriously.
A simple way to remember: If it’s red, hot, and growing—call your doctor.
Recognizing the root causes behind cellulite and cellulitis means you can spot the difference, respond quickly, and confidently ignore myths about “cleanliness” or “simple skin issues”—one is cosmetic, the other urgent.
Typical Symptoms: Side-by-Side Comparison
Cellulite: Cosmetic and Subtle Signs
Cellulite is all about skin texture changes, not infection.
When you spot dimpled, lumpy, or “orange peel” skin, you’re seeing cellulite. It pops up most often on your thighs, buttocks, or hips—imagine the surface of a foam cushion where someone’s pressed their thumb.
Most of the time, you’ll notice cellulite only when you’re standing, sitting, or pinching the skin:
- No pain, swelling, heat, or red coloring
- Skin feels and looks normal outside the textured area
- No fever, chills, or illness
- Progression is slow—if any—usually tied to body changes
Picture this: you run your hand over your thigh and feel small lumps, but there’s no discomfort or heat. That’s classic cellulite—cosmetic only, not a health danger.
Cellulitis: Red Flags for Infection
Cellulitis is the total opposite—a red, hot medical alert.
This is a bacterial skin infection, and symptoms tend to hit fast. Pay close attention if you notice:
- New redness, warmth, swelling, and pain in one spot
- Skin may look tight, shiny, or feel tender to the touch
- Changes often spread over hours or days
- Systemic warning signs: fever, chills, fatigue, swollen lymph nodes
Think of a red patch on your calf that grows larger, feels hot, and starts throbbing—plus you’re feeling under the weather. That’s a key “get checked now” scenario.
Visual cue: “If it’s red, hot, and spreading, see a doctor fast.”
Including a self-check photo or side-by-side diagram is helpful for comparing normal dimpled skin (cellulite) to angry, red, glossy skin (cellulitis).
Know What to Look For Instantly
Cellulite: Longstanding, painless, lumpy skin—rarely changes quickly.
Cellulitis: Sudden, red, swollen area that expands—often with illness.
Remember: “No pain, no fever, likely cellulite. Red, hot, and sick? Doctor time.”
If you ever spot a patch that’s spreading, hot, or associated with illness, don’t delay—prompt medical attention is vital.
Three takeaways: know the normal dimpled look, watch for new redness or heat, and trust your instincts if things change quickly. That’s how you keep yourself (and your skin) safe.
Treatments: Cosmetic vs. Medical Urgency
Cellulite: Optional Improvements
If you’re dealing with cellulite, remember it’s purely a cosmetic concern—no medical urgency required.
Modern approaches to smoothing that lumpy or “orange peel” texture span a wide range:
- Lifestyle changes: healthy eating and regular exercise help with overall fat distribution
- Massage or manual therapies: temporarily boost circulation and break up fluid
- Mechanical or laser devices: in-clinic treatments for mild smoothing—effects can fade over weeks to months
- Topical creams: caffeine-based lotions or retinoids may offer visible but short-lived results
There’s no “cure,” and even the best treatments offer partial, temporary improvements—set realistic expectations.
Curious about new methods? Emerging tech—like acoustic wave therapy or injectable devices—are gaining buzz, but long-term data is still limited.
If you’re unhappy with your cellulite’s appearance and want expert advice, consult a dermatologist or cosmetic professional.
“Cellulite won’t hurt you, but solutions are all about preference—not necessity.”
Picture this: You spend weeks using a fancy device, notice a little smoothness, but by next season, it’s back. That’s normal!
Cellulitis: When Infection Demands Action
Cellulitis is a different story—it’s a medical emergency, not a beauty issue.
The gold standard is prompt antibiotics:
- Mild cases: oral antibiotics (like cephalexin) for about 5–10 days
- Severe or rapidly spreading cases: IV antibiotics and often hospital care
Keep an eye out for these warning signs:
- Severe pain or tenderness
- Fever or chills
- Redness that’s hot, swollen, and spreading fast
- Feeling weak, dizzy, or generally unwell
Supportive steps at home include:
- Resting the affected limb
- Elevating to reduce swelling
- Taking pain relievers as needed
- Keeping the area clean and dry
Delays in treatment can lead to dangerous complications, like sepsis or tissue death—don’t risk it. If you’re unsure, play it safe and see a doctor, stat.
“If you notice red, hot, swollen skin with fever, don’t Google-treat—get medical help immediately.”
Key Takeaway
Treat cellulite if you want smoother skin, but know improvements are subtle and never urgent. For cellulitis, time is critical: antibiotics aren’t optional, and medical care can’t wait.
Remember: cosmetic tweak or urgent treatment—know what you’re dealing with, trust your gut, and when in doubt, call your doctor.
Why the Distinction Matters: Avoiding Confusion and Ensuring Proper Care
Knowing the difference between cellulite and cellulitis isn't just trivia—it's critical for your health.
Mixing up the two can have real-world consequences, especially when it comes to cellulitis, which requires urgent medical attention.
If you mistake a spreading, red, painful skin infection for harmless dimples, you could delay treatment, leading to complications like tissue death or sepsis.
Picture this: You spot a patch of bumpy skin on your thigh. Is it the classic “orange peel” effect of cellulite, or is it a hot, red, expanding area—classic warning signs of cellulitis?
Consequences of Confusing Cellulite and Cellulitis
When cellulitis is misidentified as cellulite:
- Delaying antibiotics can allow the infection to spread, risking your limb—or your life.
- A red, hot, and swollen patch ignored for even 24-48 hours can escalate to hospital-level care.
- Close to 90% of women have cellulite, but anyone can get cellulitis if bacteria enter the skin—age and gender aren’t the point, urgency is.
When cellulite is mistaken for cellulitis:
- You might face unnecessary stress, medical bills, or even take unneeded antibiotics, which can cause side effects and resistance.
- Real cosmetic concerns get sidelined in the face of false alarms.
Why Self-Diagnosis and Googling Can Be Risky
- Cellulite is long-lasting, painless, and not red or hot—don’t let online photos mislead you.
- Cellulitis can silently progress; pictures can’t capture fever or the urgency of symptoms.
- “If it’s red, hot, and spreading—get checked!” Trust your symptoms more than your search engine.
Actionable, Scannable Takeaways
Remember these key cues:
- Cellulite: Dimpled, “orange peel” skin. No pain, fever, or redness. Cosmetic only.
- Cellulitis: Sudden, red, hot, swollen, painful. May have fever and feel sick. Needs urgent care.
If you’re not sure, or symptoms are changing—see a doctor. Trust timely action over hoping for the best.
When you know the cues, you’ll protect your health and get the right care, fast. For more help, check our detailed symptom checklists and risk assessment tools linked below.
Conclusion
Spotting the real difference between cellulite and cellulitis is about more than trivia—it’s about protecting your health and your peace of mind. With a quick, confident check, you can avoid panic in the mirror or, more importantly, get rapid care when it truly counts.
When you’re able to tell cosmetic from critical, you step into the driver’s seat—empowered to skip needless worry or react fast if warning signs appear.
Key takeaways you can use right away:
- Trust what you see and feel: If your skin is suddenly red, hot, swollen, or painful—with or without fever—seek medical care promptly.
- Cosmetic changes only? Dimples, lumps, and “orange peel” texture (without pain or redness) are almost always just cellulite—treat only if you want to, not because you have to.
- Don’t rely on Google images alone: Pair what you see with your symptoms. Listen to your body first, not just search results.
- When in doubt, act now: Uncertainty about a new skin patch? Reach out to a healthcare provider—it’s never too cautious.
Next steps for you:
- Do a quick skin scan today—know your normal, so you spot changes before they escalate.
- Save or share this guide for easy reference and to help others cut through confusion.
- Bookmark symptom checklists or create a note on your phone with early warning signs, so you won’t hesitate if the need arises.
Clear knowledge is power—and your best tool against panic or delay. Make each skin check a small act of self-advocacy.
Trust yourself, respond quickly when it matters, and remember: confidence starts with understanding, not guessing.
Your awareness might be the fastest cure there is.